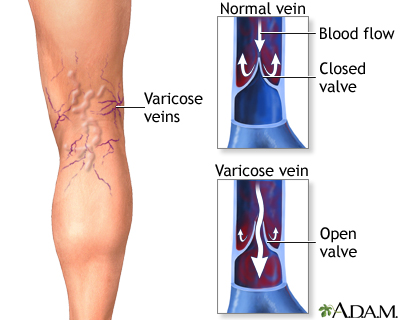
Varicose veins are swollen, twisted, and enlarged veins that you can see under the skin. They are often red or blue in color. They most often appear in the legs, but can occur in other parts of the body.
Causes
Normally, one-way valves in your leg veins keep blood moving up toward the heart. When the valves do not work properly, they allow blood to back up into the vein. The vein swells from the blood that collects there, which causes varicose veins over time.
Varicose veins are common, and affect more women than men. They do not cause problems for most people. However, if the flow of blood through veins becomes poor enough, problems such as leg swelling and pain, blood clots, and skin changes may be present.
Risk factors include:
- Older age
- Being female (hormonal changes from puberty, pregnancy, and menopause can lead to varicose veins, and taking birth control pills or hormone replacement can increase your risk)
- Being born with defective valves in the veins
- Obesity
- Pregnancy
- History of blood clots in your legs
- Standing or sitting for long periods of time
- Family history of varicose veins
Symptoms
Symptoms of varicose veins include:
- Fullness, heaviness, aching, and sometimes pain in the legs
- Visible, swollen veins
- Very small veins that you can see on the surface of the skin, called spider veins.
- Thigh or calf cramps (often at night)
- Mild swelling of feet or ankles
- Itching near the varicose veins
- Restless leg symptoms
If flow of blood through the veins becomes poor enough, symptoms may include:
- Leg swelling
- Leg or calf pain after sitting or standing for long periods
- Skin color changes of the legs or ankles
- Dry, irritated, scaly skin that can crack easily
- Skin sores (ulcers) that do not heal easily
- Thickening and hardening of the skin in the legs and ankles (this can happen over time)
Exams and Tests
Your health care provider will examine your legs to look for swelling, changes in skin color, or sores. Your provider also may:
- Check blood flow in the veins
- Check for other problems with the legs (such as a blood clot)
Treatment
Your provider may suggest that you take the following self-care steps to help manage varicose veins:
- Wear compression stockings to decrease swelling. These stockings gently squeeze your legs to move blood up toward your heart.
- DO NOT sit or stand for long periods. Even moving your legs slightly helps keep the blood flowing.
- Raise your legs above your heart 3 or 4 times a day for 15 minutes at a time.
- Care for wounds if you have any open sores or infections. Your provider can show you how.
- Lose weight if you are overweight.
- Get more exercise. This can help you keep off weight and help move blood up your legs. Walking or swimming are good options.
- If you have dry or cracked skin on your legs, moisturizing may help. However, some skin care treatments can make the problem worse. Talk to your provider before using any lotions, creams, or antibiotic ointments. Your provider can recommend lotions that can help.
If only a small number of varicose veins are present, the following procedures may be used:
- Sclerotherapy. Salt water or a chemical solution is injected into the vein. The vein hardens and disappears.
- Phlebectomy. Small surgical cuts are made in the leg near the damaged vein. The vein is removed through one of the cuts.
- If the varicose veins are larger, longer, or more widespread on the leg, your provider will suggest a procedure using such a laser or radiofrequency, which can be done in the provider's office or clinic.
Outlook (Prognosis)
Varicose veins tend to get worse over time. Taking self-care steps can help relieve achiness and pain, keep varicose veins from getting worse, and prevent more serious problems.
When to Contact a Medical Professional
Contact your provider if:
- Varicose veins are painful.
- They get worse or do not improve with self-care, such as by wearing compression stockings or avoiding standing or sitting for too long.
- You have a sudden increase in pain or swelling, fever, redness of the leg, or leg sores.
- You develop leg sores that do not heal.
Alternative Names
Varicosity
Patient Instructions
Images
References
Iafrati MD. Varicose veins: surgical treatment. In: Sidawy AN, Perler BA, eds. Rutherford's Vascular Surgery and Endovascular Therapy. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 154.
Pascarella L, Marston W. Venous disease. In: Townsend CM Jr, Beauchamp RD, Evers BM, Mattox KL, eds. Sabiston Textbook of Surgery. 21st ed. St Louis, MO: Elsevier; 2022:chap 65.
Sadek M, Kabnick LS. Varicose veins: endovenous ablation and sclerotherapy. In: Sidawy AN, Perler BA, eds. Rutherford's Vascular Surgery and Endovascular Therapy. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 155.
Review Date 5/10/2024
Updated by: Neil Grossman, MD, Saint Vincent Radiological Associates, Framingham, MA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.