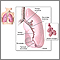
Byssinosis is a disease of the lungs. It is caused by breathing in (inhaling) cotton dust or dusts from other vegetable fibers such as flax, hemp, or sisal while at work.
Causes
Inhaling the dust produced by raw cotton can cause byssinosis. It is most common in people who work in the textile industry.
Those who are sensitive to the dust can have an asthma-like condition after being exposed.
Methods of prevention in the United States have reduced the number of cases. Byssinosis is still common in developing countries. Smoking increases risk of developing this disease. Being exposed to the dust many times can lead to long-term (chronic) lung disease.
Exams and Tests
Your health care provider will take your medical history. You'll be asked if your symptoms relate to certain exposures or times of exposure. Your provider will also do a physical exam, paying special attention to the lungs.
Tests that may be ordered include:
Treatment
The most important treatment is to stop being exposed to the dust. Reducing dust levels in the factory (by improving machinery or ventilation) will help prevent byssinosis. Some people may have to change jobs to avoid further exposure.
Medicines used for asthma, such as bronchodilators, usually improve symptoms. Corticosteroid medicines may be prescribed in more severe cases.
Stopping smoking is very important for people with this condition. Breathing treatments, including nebulizers, may be prescribed if the condition becomes long-term. Home oxygen therapy may be needed if blood oxygen level is low.
People with a long-term (chronic) lung disease can be helped with:
- Physical exercise programs
- Breathing exercises
- Patient education programs
Outlook (Prognosis)
Stopping exposure to the dust often improves symptoms. Continued exposure can lead to reduced lung function. In the United States, worker's compensation may be available to people with byssinosis.
Possible Complications
Chronic bronchitis may develop. This is swelling (inflammation) of the large airways of the lungs with a large amount of phlegm production. Continued exposure can lead to end-stage lung disease.
When to Contact a Medical Professional
Contact your provider if you suspect that you have been exposed to cotton or other fiber dust at work and you have breathing problems. Having byssinosis makes it easier for you to develop lung infections.
If you've been diagnosed with byssinosis, contact your provider right away if you develop a cough, shortness of breath, fever, or other signs of a lung infection, especially if you think you have the flu. Since your lungs are already damaged, it's very important to have the infection treated right away. This will prevent breathing problems from becoming severe, as well as further damage to your lungs.
Talk to your provider about getting the flu, pneumonia (pneumococcal), and other recommended vaccines.
Prevention
Controlling dust, using face masks, and other measures can reduce the risk. Stop smoking, especially if you work in textile manufacturing.
Alternative Names
Cotton worker's lung; Cotton bract disease; Mill fever; Brown lung disease; Monday fever
Images
References
Go LHT, Cohen RA. Pneumoconioses. In: Broaddus VC, Ernst JD, King TE, et al, eds. Murray and Nadel's Textbook of Respiratory Medicine. 7th ed. Philadelphia, PA: Elsevier; 2022:chap 101.
Tarlo SM, Redlich CA. Occupational lung disease. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 81.
Review Date 4/10/2025
Updated by: Allen J. Blaivas, DO, Division of Pulmonary, Critical Care, and Sleep Medicine, VA New Jersey Health Care System, Clinical Assistant Professor, Rutgers New Jersey Medical School, East Orange, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.