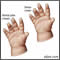
Fetal alcohol spectrum disorders (FASD) are groupings of growth, mental, and physical problems that may occur in a baby when a mother drinks alcohol during pregnancy. Fetal alcohol syndrome (FAS) is the most severe form of FASD.
Causes
Using alcohol during pregnancy can cause the same risks as using alcohol in general. But it poses extra risks to an unborn baby. When a pregnant woman drinks alcohol, it easily passes across the placenta to the fetus. Because of this, drinking alcohol can harm an unborn baby.
There is no safe level of alcohol use during pregnancy. Larger amounts of alcohol appear to increase the problems. Binge drinking is more harmful than drinking small amounts of alcohol.
Timing of alcohol use during pregnancy is also important. Drinking alcohol is likely most harmful during the first 3 months of pregnancy. But drinking alcohol any time during pregnancy can be harmful.
Symptoms
A baby with FAS may have the following symptoms:
- Poor growth while the baby is in the womb and after birth
- Decreased muscle tone and poor coordination
- Delayed developmental milestones
- Vision difficulties, such as nearsightedness (myopia)
- Hyperactivity
- Anxiety
- Extreme nervousness
- Short attention span
Exams and Tests
A physical exam of the baby may show a heart murmur or other heart problems. A common defect is a hole in the wall that separates the right and left lower chambers (ventricles) of the heart.
There also may be problems with the face and bones. These may include:
- Narrow and small eyes
- Small head and upper jaw
- Smooth groove in the upper lip or smooth and thin upper lip
- Deformed ears
- Flat, short, and upturned nose
- Ptosis (drooping of upper eyelids)
Tests that may be done include:
- Blood alcohol level in pregnant women who show signs of being drunk (intoxicated)
- Brain imaging tests (CT or MRI) after the child is born
- Pregnancy ultrasound
Treatment
Women who are pregnant or who are trying to get pregnant should not drink any amount of alcohol. Pregnant women with alcohol use disorder should join a rehab program and be checked closely by their health care provider throughout their pregnancy.
Outlook (Prognosis)
The outcome for infants with FAS varies. Almost none of these babies have normal brain development.
Infants and children with FAS have many different problems, which can be difficult to manage. Children do best if they are diagnosed early and referred to a team of providers who can work on educational and behavioral strategies that fit the child's needs.
When to Contact a Medical Professional
Contact your provider for an appointment if you are drinking alcohol regularly or heavily, and are finding it difficult to cut back or stop. Also contact your provider if you are drinking alcohol in any amount while you are pregnant or trying to get pregnant.
Prevention
Avoiding alcohol during pregnancy prevents FAS. Counseling can help women who have already had a child with FAS.
Sexually active women who drink heavily should use birth control and control their drinking behaviors, or stop using alcohol before trying to get pregnant.
Alternative Names
Alcohol in pregnancy; Alcohol-related birth defects; Fetal alcohol effects; FAS; Fetal alcohol spectrum disorders; Alcohol abuse - fetal alcohol; Alcoholism - fetal alcohol
References
Friedman SA, Hurt H. Fetal alcohol spectrum disorder. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 146.
Hoyme HE, Kalberg WO, Elliott AJ, et al. Updated clinical guidelines for diagnosing fetal alcohol spectrum disorders. Pediatrics. 2016;138(2):e20154256. PMID: 27464676 pubmed.ncbi.nlm.nih.gov/27464676/.
Weber RJ, Jauniaux ERM. Drugs and environmental agents in pregnancy and lactation: teratology, epidemiology, and patient management. In: Landon MB, Galan HL, Jauniaux ERM, et al, eds. Gabbe's Obstetrics: Normal and Problem Pregnancies. 8th ed. Philadelphia, PA: Elsevier; 2021:chap 7.
Review Date 7/16/2024
Updated by: Neil K. Kaneshiro, MD, MHA, Clinical Professor of Pediatrics, University of Washington School of Medicine, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.