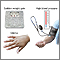
HELLP syndrome is a group of symptoms that occur in pregnant women who have:
- H: hemolysis (the breakdown of red blood cells)
- EL: elevated liver enzymes
- LP: low platelet count
Causes
The cause of HELLP syndrome has not been found. It is considered to be a variant of preeclampsia. Sometimes the presence of HELLP syndrome is due to an underlying disease, such as antiphospholipid antibody syndrome.
HELLP syndrome occurs in about 1 to 2 out of 1,000 pregnancies. In women with preeclampsia or eclampsia, the condition develops in 10% to 20% of pregnancies.
Risk factors for HELLP syndrome include:
- Age greater than 35
- Obesity (metabolic syndrome)
- History of preeclampsia
- History of diabetes or renal disease
- History of multiple births
- History of high blood pressure
Most often, HELLP develops during the third trimester of pregnancy (between 26 to 40 weeks gestation). Sometimes it develops in the week after the baby is born.
Many women have high blood pressure and are diagnosed with preeclampsia before they develop HELLP syndrome. In some cases, HELLP symptoms are the first warning of preeclampsia. The condition is sometimes misdiagnosed as:
- Flu or other viral illness
- Gallbladder disease
- Hepatitis
- Idiopathic thrombocytopenic purpura (ITP)
- Lupus flare
- Thrombotic thrombocytopenic purpura
Exams and Tests
During a physical exam, the health care provider may discover:
- Abdominal tenderness, especially in the right upper side
- Enlarged liver
- High blood pressure
- Swelling in the legs
Liver function tests (liver enzymes) may be high. Platelet counts may be low. A CT scan may show bleeding into the liver. Excessive protein (proteinuria) may be found in the urine.
Tests of the baby's health will be done. Tests include fetal non-stress test and ultrasound, among others.
Treatment
The main treatment is to deliver the baby as soon as possible, even if the baby is premature. Problems with the liver and other complications of HELLP syndrome can quickly get worse and be harmful to both the mother and child.
Your provider may induce labor by giving you medicines to start labor, or may perform a C-section.
You may also receive:
- A blood transfusion if bleeding problems become severe
- Corticosteroid medicines to help the baby's lungs develop faster
- Medicines to treat high blood pressure
- Magnesium sulfate infusion to prevent seizures
Outlook (Prognosis)
Outcomes are most often good if the problem is diagnosed early. It is very important to have regular prenatal checkups. You should also let your provider know right away if you have symptoms of this condition.
When the condition is not treated early, up to 1 of 4 women develop serious complications. Without treatment, a small number of women die.
The death rate among babies born to mothers with HELLP syndrome depends on birth weight and the development of the baby's organs, especially the lungs. Many babies are born prematurely (born before 37 weeks of pregnancy).
HELLP syndrome may return in up to 1 out of 4 future pregnancies.
Possible Complications
There can be complications before and after the baby is delivered, including:
- Disseminated intravascular coagulation (DIC). A clotting disorder that leads to excess bleeding (hemorrhage).
- Fluid in the lungs (pulmonary edema).
- Kidney failure.
- Liver hemorrhage and failure.
- Separation of the placenta from the uterine wall (placental abruption).
- Seizures.
- Stroke.
- Fetal complications, including restriction of fetal growth.
After the baby is born, HELLP syndrome goes away in most cases in 2 to 3 days.
When to Contact a Medical Professional
If symptoms of HELLP syndrome occur during pregnancy:
- See your provider right away.
- Call 911 or the local emergency number.
- Get to the hospital emergency room or labor and delivery unit.
There is no known way to prevent HELLP syndrome. All pregnant women should start prenatal care early and continue it through the pregnancy. This allows the provider to find and treat conditions such as HELLP syndrome right away.
Images
References
Bartal MF, Costantine M, Sibai B. Hypertensive disorders of pregnancy. In: Landon MB, Galan HL, Jauniaux ERM, et al, eds. Gabbe's Obstetrics: Normal and Problem Pregnancies. 9th ed. Philadelphia, PA: Elsevier; 2025:chap 38.
Mehra S, Reinus JF. Gastrointestinal and hepatic disorders in the pregnant patient. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 40.
Review Date 10/15/2024
Updated by: John D. Jacobson, MD, Professor Emeritus, Department of Obstetrics and Gynecology, Loma Linda University School of Medicine, Loma Linda, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.