Allergic rhinitis is a diagnosis associated with a group of symptoms affecting the nose. These symptoms occur when you breathe in something you are allergic to, such as dust, animal dander, or pollen. Symptoms can also occur when you eat a food that you are allergic to.
This article focuses on allergic rhinitis due to plant pollens. This type of allergic rhinitis is commonly called hay fever. It is also called seasonal allergies because it may occur only during certain seasons.
Causes
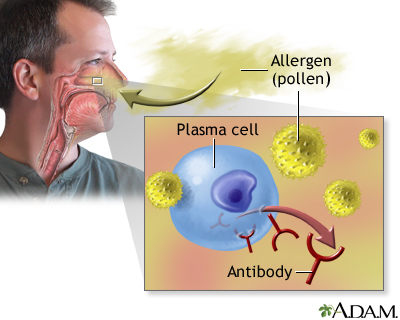
An allergen is something that triggers an allergy. When a person with allergic rhinitis breathes in an allergen such as pollen, mold, animal dander, or dust, the body releases chemicals that cause allergy symptoms.
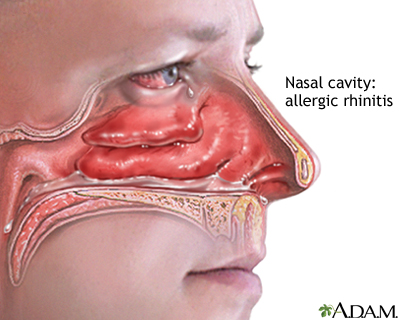
Hay fever involves an allergic reaction to pollen.
Plants that cause hay fever are trees, grasses, and ragweed. Their pollen is carried by the wind. Flower pollen is carried by insects and does not cause hay fever. Types of plants that cause hay fever vary from person to person and from area to area.
The amount of pollen in the air can affect whether hay fever symptoms develop or not.
- Hot, dry, windy days are more likely to have a lot of pollen in the air.
- On cool, damp, rainy days, most pollen is washed to the ground.
Hay fever and allergies often run in families. If both of your parents have hay fever or other allergies, you are likely to have hay fever and allergies, too. The chance is higher if your mother has allergies.
Symptoms
Symptoms that occur shortly after you come into contact with the substance you are allergic to may include:
- Itchy nose, mouth, eyes, throat, skin, or any area
- Problems with smell
- Runny nose
- Sneezing
- Watery eyes
Symptoms that may develop later include:
- Stuffy nose (nasal congestion)
- Coughing
- Clogged ears and decreased sense of smell
- Sore throat
- Dark circles under the eyes
- Puffiness under the eyes
- Fatigue and irritability
- Headache
Exams and Tests
Your health care provider will perform a physical exam and ask about your symptoms. You will be asked whether your symptoms vary by time of day or season, and exposure to pets or other allergens.
Allergy testing may reveal the pollen or other substances that trigger your symptoms. Skin testing is the most common method of allergy testing.
If your provider determines you cannot have skin testing, special blood tests may help with the diagnosis. These tests, known as IgE RAST tests, can measure the levels of allergy-related substances.
A blood test, called the eosinophil count, may also help diagnose allergies.
Treatment
LIFESTYLE AND AVOIDING ALLERGENS
The best treatment is to avoid the pollens that cause your symptoms. It may be impossible to avoid all pollen. But you can often take steps to reduce your exposure.
You may be prescribed medicine to treat allergic rhinitis. The medicine your provider prescribes depends on your symptoms and how severe they are. Your age and whether you have other medical conditions, such as asthma, will also be considered.
For mild allergic rhinitis, a nasal wash can help remove mucus from the nose. You can buy a saline solution at a drug store or make one at home using 1 cup (c) or 237 milliliters (ml) of distilled or boiled then cooled water, half a teaspoon (tsp) or 3 grams (g) of salt, and a pinch of baking soda.
Treatments for allergic rhinitis include:
ANTIHISTAMINES
Medicines called antihistamines work well for treating allergy symptoms. They may be used when symptoms do not happen often or do not last long. Be aware of the following:
- Many antihistamines taken by mouth can be bought without a prescription.
- Some antihistamines can cause sleepiness. You should not drive or operate machines after taking this type of medicine.
- Others antihistamines cause little or no sleepiness.
- Antihistamine nasal sprays work well for treating allergic rhinitis. Ask your provider if you should try these medicines first.
- Antihistamine eye drops can be used as needed for itchy, watery eyes.
CORTICOSTEROIDS
- Nasal corticosteroid sprays are the most effective treatment for allergic rhinitis. They work best when used nonstop, but they can also be helpful when used for shorter periods of time. They can even help when used intermittently.
- Corticosteroid sprays are generally safe for children and adults.
- Many brands are available without a prescription. For specific brands, you may need a prescription from your provider.
DECONGESTANTS
- Decongestants may also be helpful for reducing symptoms such as nasal stuffiness.
- Do not use nasal spray decongestants for more than 3 days.
OTHER MEDICINES
- Leukotriene inhibitors are prescription medicines that block leukotrienes. These are some of the chemicals the body releases in response to an allergen that also trigger symptoms. These medicines can cause side effects such as anxiety or depression in some people. Speak with your provider before starting these medications if you have a history of mental health issues.
ALLERGY SHOTS
Allergy shots (immunotherapy) are sometimes recommended if you cannot avoid the pollen and your symptoms are hard to control. This includes regular shots of the pollen you are allergic to. Each dose is slightly larger than the dose before it, until you reach the dose that helps control your symptoms. Allergy shots may help your body adjust to the pollen that is causing the reaction.
SUBLINGUAL IMMUNOTHERAPY TREATMENT (SLIT)
Instead of shots, medicine put under the tongue may help for dust, grass and ragweed allergies.
Outlook (Prognosis)
Most symptoms of allergic rhinitis can be treated with medicines. More severe cases need allergy shots.
Some people, especially children, may outgrow an allergy as the immune system becomes less sensitive to the trigger. But once a substance such as pollen causes allergies, it often continues to have a long-term effect on the person.
When to Contact a Medical Professional
Contact your provider for an appointment if:
- You have severe hay fever symptoms
- Treatment that once worked for you no longer works
- Your symptoms do not respond to treatment
Prevention
You can sometimes prevent symptoms by avoiding the pollen you are allergic to. During pollen season, you should stay indoors where it is air-conditioned, if possible. Sleep with the windows closed, and drive with the windows rolled up.
Alternative Names
Hay fever; Nasal allergies; Seasonal allergy; Seasonal allergic rhinitis; Allergies - allergic rhinitis; Allergy - allergic rhinitis
References
Corren J, Baroody FM, Togias A. Allergic and nonallergic rhinitis. In: Burks AW, Holgate ST, O'Hehir RE, et al, eds. Middleton's Allergy: Principles and Practice. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 40.
Custovic A, Tovey E. Allergen control for prevention and management of allergic diseases. In: Burks AW, Holgate ST, O'Hehir RE, et al, eds. Middleton's Allergy: Principles and Practice. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 84.
Liu AH, Bacharier LB, Fitzpatrick AM, Sicherer SH. Childhood asthma. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 185.
Nadeau KC. Approach to the patient with allergic or immunologic disease. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 230.
Sylvester MJ, Wise SK, Baroody FM. Allergy and immunology of the upper airway. In: Francis HW, Haughey BH, Hillel AT, et al, eds. Cummings Otolaryngology: Head & Neck Surgery. 8th ed. Philadelphia, PA: Elsevier; 2026:chap 34.
Review Date 1/20/2026
Updated by: Deborah Pedersen, MD, MS, Allergy & Asthma Care, PC, Taunton, MA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.