A herniated (slipped) disk occurs when all or part of a disk is forced through a weakened part of the disk. This may place pressure on nearby nerves or the spinal cord.
Causes
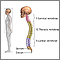
The bones (vertebrae) of the spinal column protect nerves that come out of the brain and travel down your back to form the spinal cord. Nerve roots are large nerves that branch out from the spinal cord and leave your spinal column between each vertebra.
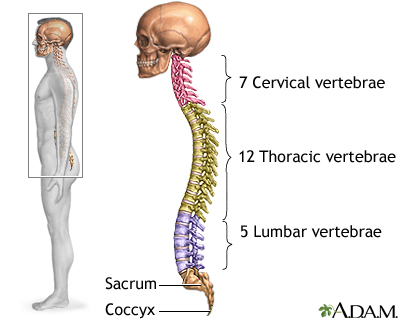
The spinal bones are separated by disks. These disks cushion the spinal column and put space between your vertebrae. The disks allow movement between the vertebrae, which lets you bend and reach.
With herniated disk:
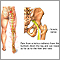
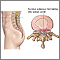
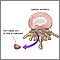
- The disk may move out of place (herniate) or break open (rupture) from injury or strain. When this happens, there may be pressure on one or more spinal nerves. This can lead to pain, numbness, or weakness.
- The lower back (lumbar area) of the spine is the most common area affected by a herniated disk. The neck (cervical) disks are the second most commonly affected area. The upper-to-mid-back (thoracic) disks are rarely involved.
A herniated disk is a cause of radiculopathy. This is a condition that affects one or more of the spinal nerve roots.
Herniated disks occur more often in middle-aged and older men, usually after strenuous activity. Other risk factors may include:
- Lifting heavy objects
- Being overweight
- Repetitive bending or twisting the lower back or neck
- Sitting or standing in same position for long hours
- Inactive lifestyle
- Smoking
 Watch this video about:Herniated nucleus pulposus (slipped disk)
Watch this video about:Herniated nucleus pulposus (slipped disk)Symptoms
The pain most often occurs on one side of the body. Symptoms vary, depending on the site of injury, and may include the following:
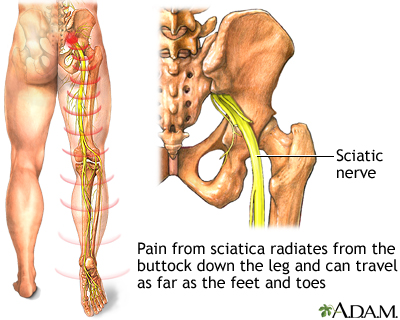
- With a herniated disk in your lower back, you may have sharp pain in one part of the leg, hip, or buttocks, and numbness in other parts. You may also feel pain or numbness in the back of the calf or sole of the foot. The same leg may also feel weak.
- With a herniated disk in your neck, you may have pain when moving your neck, deep pain near or over the shoulder blade, or pain that moves to the upper arm, forearm, and fingers. You can also have numbness along your shoulder, elbow, forearm, and fingers.
The pain often starts slowly. It may get worse:
- After standing or sitting
- At night
- When sneezing, coughing, or laughing
- When bending backward or walking more than a few yards or meters
- When straining or holding your breath, such as when having a bowel movement
You may also have weakness in certain muscles. Sometimes, you may not notice it until your health care provider examines you. In other cases, you will notice that you have a hard time lifting your leg or arm, standing on your toes on one side, squeezing tightly with one of your hands, or other problems. You may lose control of your bladder or bowels.
The pain, numbness, or weakness often goes away or improves a lot over weeks to months.
Exams and Tests
A careful physical exam and history is the first step. Depending on where you have symptoms, your provider examines your neck, shoulder, arms, and hands, or your lower back, hips, legs, and feet.
Your provider will check:
- For numbness or loss of feeling
- Your muscle reflexes, which may be slower or missing
- Your muscle strength, which may be weaker
- Your posture, or the way your spine curves
- Your ability to flex your spine
Your provider may also ask you to:
- Sit, stand, and walk. While you walk, your provider may ask you to try walking on your toes and then your heels.
- Bend forward, backward, and sideways.
- Move your neck forward, backward, and sideways.
- Raise your shoulders, elbow, wrist, and hand, and check your strength during these tasks.
Leg pain that occurs when you sit on an exam table and lift your leg straight up usually suggests a herniated disk in your lower back.
In another test, you will bend your head forward and to the sides while the provider puts slight downward pressure on the top of your head. Increased pain or numbness during this test is usually a sign of pressure on a nerve in your neck.
DIAGNOSTIC TESTS
Tests that may be done may include:
- Spine MRI or spine CT to show where the herniated disk is pressing on the spinal canal.
- Electromyography (EMG) to determine the exact spinal nerve root that is involved.
- Myelogram to determine the size and location of disk herniation.
- Nerve conduction velocity test.
- Spine x-ray to check for other causes of back or neck pain. It can look at how healthy your bone is and also look for how much room there is for your spinal nerves to travel out of the spinal cord. However, it is not possible to diagnose a herniated disk by a spine x-ray alone.
- Bone density tests to check your bone quality. If your bone is weak, you may be given medicine to improve bone health.
Treatment
The first treatment for a slipped disk is a short period of rest and taking medicines for the pain. This is usually followed by physical therapy. Most people who follow these treatments recover and return to normal activities. Some people will need to have more treatment. This may include steroid injections or surgery.
MEDICINES
Medicines can help with your pain. Your provider may prescribe any of the following:
- Nonsteroidal anti-inflammatory drugs (NSAIDs) for long-term pain control
- Narcotics if the pain is severe and does not respond to NSAIDs
- Medicines to calm the nerves
- Muscle relaxants to relieve back spasms
LIFESTYLE CHANGES
If you are overweight, diet and exercise are very important for improving back pain.
Physical therapy is important for nearly everyone with disk disease. Therapists will teach you how to properly lift, dress, walk, and perform other activities. They will teach you how to strengthen muscles that help support the spine. You will also learn how to increase flexibility in your spine and legs.
Take care of your back at home:
- Reduce activity for the first few days. Slowly restart your usual activities.
- Avoid heavy lifting or twisting your back for the first 6 weeks after the pain starts.
- After 2 to 3 weeks, gradually start exercising again.
INJECTIONS
Steroid medicine injections into the back in the area of the herniated disk may help control pain for several months. These injections reduce swelling around the spinal nerve and disk and relieve many symptoms. They do not solve the underlying problem and your pain may return after weeks or months. Spinal injections are an outpatient procedure.
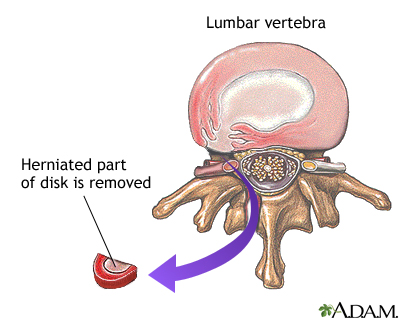
SURGERY
Surgery may be an option if your symptoms do not go away with other treatments and time.
One such surgery is diskectomy, which removes all or part of a disk.
Discuss with your provider which treatment options are best for you.
Outlook (Prognosis)
Most people improve with treatment. But you may have long-term back pain, even after treatment.
It may take several months to a year or more to go back to all of your activities without having pain or straining your back. People who work in jobs that involve heavy lifting or back strain may need to change their job activities to avoid injuring their back again.
Possible Complications
In rare cases, the following problems can occur:
- Long-term back pain or leg pain
- Loss of movement or feeling in the legs or feet
- Loss of bowel or bladder function
- Permanent spinal cord injury (very rare)
When to Contact a Medical Professional
Contact your provider if you have:
- Severe back pain that does not go away
- Any numbness, loss of movement, weakness, or bowel or bladder changes
Prevention
To help prevent back injury:
- Use proper lifting techniques.
- Maintain a healthy weight.
- Do exercises to keep your abdominal (core) and back muscles strong.
- Evaluate your setup at work. Sometimes a standing desk or changing the location of your computer screen can help your condition.
Your provider may suggest a back brace to help support the spine. A brace may prevent injuries in people who lift heavy objects at work. But using these devices too much can weaken the muscles that support your spine and make the problem worse.
Alternative Names
Lumbar radiculopathy; Cervical radiculopathy; Herniated intervertebral disk; Prolapsed intervertebral disk; Slipped disk; Ruptured disk; Herniated nucleus pulposus; Low back pain - herniated disk; LBP - herniated disk; Sciatica - herniated disk; Herniated disk; Disc - herniated
References
Farrell SE, Ma ZB. Musculoskeletal back pain. In: Walls RM, eds. Rosen's Emergency Medicine: Concepts and Clinical Practice. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 104.
Gardocki RJ, Park AL. Degenerative disorders of the thoracic and lumbar spine. In: Azar FM, Beaty JH, eds. Campbell's Operative Orthopaedics. 14th ed. Philadelphia, PA: Elsevier; 2021:chap 39.
Magee DJ, Manske RC. Lumbar spine. In: Magee DJ, Manske RC, eds. Orthopedic Physical Assessment. 7th ed. St Louis, MO: Elsevier; 2021:chap 9.
Review Date 8/27/2024
Updated by: C. Benjamin Ma, MD, Professor, Chief, Sports Medicine and Shoulder Service, UCSF Department of Orthopaedic Surgery, San Francisco, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.