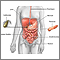
Salmonella enterocolitis is a bacterial infection in the lining of the small intestine that is caused by Salmonella bacteria. It is a type of food poisoning.
Causes
Salmonella infection is one of the most common types of food poisoning. It occurs when you eat food or drink water that contains Salmonella bacteria.
The Salmonella bacteria may get into the food you eat in several ways.
You are more likely to get this type of infection if you:
- Eat foods such as turkey, turkey dressing, chicken, or eggs that have not been cooked well or stored properly
- Are around family members with a recent Salmonella infection
- Have been in or worked in a hospital, nursing home, or other long-term health facility
- Have a pet iguana or other lizards, turtles, or snakes (reptiles and amphibians can be carriers of Salmonella)
- Handle live poultry
- Have a weakened immune system
- Regularly used medicines that block acid production in the stomach
- Have Crohn disease or ulcerative colitis
- Used antibiotics in the recent past
Symptoms
The time between getting infected and having symptoms is 8 to 72 hours. Symptoms include:
- Abdominal pain, cramping, or tenderness
- Chills
- Diarrhea
- Fever
- Muscle pain
- Nausea
- Vomiting
Exams and Tests
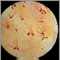
Your health care provider will perform a physical exam. You may have a tender abdomen and develop tiny pink spots, called rose spots, on your skin.
Tests that may be done include:
- Blood culture
- Complete blood count with differential
- Test for specific antibodies called febrile/cold agglutinins
- Stool culture for Salmonella
- Examination of stool for white blood cells
Treatment
The goal is to make you feel better and avoid dehydration. Dehydration means your body does not have as much water and fluids as it should.
These things may help you feel better if you have diarrhea:
- Drink 8 to 10 glasses of clear fluids every day. Water is best.
- Drink at least 1 cup (240 milliliters) of liquid every time you have a loose bowel movement.
- Eat small meals throughout the day instead of 3 big meals.
- Eat some salty foods, such as pretzels, soup, and sports drinks.
- Eat some high-potassium foods, such as bananas, potatoes without the skin, and watered-down fruit juices.
If your child has Salmonella, it is important to keep them from getting dehydrated. At first, try 1 ounce (2 tablespoons or 30 milliliters) of fluid every 30 to 60 minutes.
- Infants should continue to breastfeed and receive electrolyte replacement solutions as recommended by your child's provider.
- You can use an over-the-counter drink, such as Pedialyte or Infalyte. Do not water down these drinks.
- You can also try Pedialyte freezer pops.
- Watered-down fruit juice or broth may also help.
Medicines that slow diarrhea are often not given because they may make the infection last longer. If you have severe symptoms, your provider may prescribe antibiotics if you:
- Have diarrhea more than 9 or 10 times per day
- Have a high fever
- Need to be in the hospital
People who take diuretics ("water pills") may need to stop taking these medicines if they have acute Salmonella enteritis. Never stop taking any medicine without first talking to your provider.
Outlook (Prognosis)
In otherwise healthy people, symptoms should go away in 2 to 5 days, but they may last for 1 to 2 weeks.
People who have been treated for Salmonella may continue to shed the bacteria in their stool for months to a year after the infection. Food handlers who carry Salmonella in their body can pass the infection to the people who eat the food they have handled.
When to Contact a Medical Professional
Contact your provider if:
- There is blood or pus in your stools.
- You have diarrhea and are unable to drink fluids due to nausea or vomiting.
- You have a fever above 101°F (38.3°C) and diarrhea.
- You have signs of dehydration (thirst, dizziness, lightheadedness).
- You have recently traveled to a foreign country and developed diarrhea.
- Your diarrhea does not get better in 5 days, or it gets worse.
- You have severe abdominal pain.
Contact your provider if your child has:
- A fever above 100.4°F (38°C) and diarrhea
- Diarrhea that does not get better in 2 days, or it gets worse
- Been vomiting for more than 12 hours (in a newborn under 3 months, you should call as soon as vomiting or diarrhea begins)
- Reduced urine output, sunken eyes, sticky or dry mouth, or no tears when crying
Prevention
Learning how to prevent food poisoning can reduce the risk for this infection. Follow these safety measures:
- Properly handle and store foods.
- Wash your hands when handling eggs, poultry, and other foods.
- If you own a reptile, wear gloves when handling the animal or its feces because Salmonella can easily pass to humans.
Alternative Names
Salmonellosis; Nontyphoidal salmonella; Food poisoning - salmonella; Gastroenteritis - salmonella
References
Crump JA. Salmonella infections (including enteric fever). In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 284.
Fleckenstein JM. Approach to the patient with suspected enteric infection. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 262.
Hammershaimb EA, Kotloff KL. Acute gastroenteritis in children. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 387.
Lima AAM, Warren CA, Guerrant RL. Acute dysentery syndromes (diarrhea with fever). In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 99.
Melia JMP, Sears CL. Infectious enteritis and proctocolitis. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 110.
Review Date 3/16/2024
Updated by: Jatin M. Vyas, MD, PhD, Roy and Diana Vagelos Professor in Medicine, Columbia University Vagelos College of Physicians and Surgeons, Division of Infectious Diseases, Department of Medicine, New York, NY. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.