Eye emergencies include cuts, scratches, objects in the eye, burns, chemical exposure, and blunt injuries to the eye or eyelid. Certain eye infections and other medical conditions, such as clots or blockages of the blood vessels of the eye or glaucoma, may also need medical care right away. Since the eye is easily damaged, any of these conditions can lead to vision loss if untreated.
Considerations
It is important to get medical attention for eye or eyelid injuries and problems. Eye problems (such as a painful red eye or vision loss) that are not due to injury also need urgent medical attention.
 Watch this video about:Corneal injury
Watch this video about:Corneal injuryCauses
Eye emergencies include any of the following:
BLUNT TRAUMA
- Blunt trauma to the eye or face often causes bleeding under the skin that leaves a bruise called a "black eye." The tissue around the eye turns black and blue, gradually becoming purple, green, and yellow over several days as the blood is absorbed. The abnormal color disappears within 2 weeks.
- Swelling of the eyelid and tissue around the eye may also occur. Sometimes, serious damage to the eye itself occurs from the pressure of a swollen eyelid or face.
- Certain types of skull fractures can cause bruising around the eyes, even without direct injury to the eye.
- Common causes of blunt trauma include things like fists, tennis balls, and airbags.
- Blunt trauma can cause a hyphema, which is blood inside the front of the eye. The blood may block your view of the iris and pupil.
PENETRATING TRAUMA
- Penetrating trauma may be caused by things such as knives, ice picks, sticks, nails, and gun shots.
- Injuries can be serious and usually require repair by a surgeon. Loss of the eye is not uncommon in serious injuries.
- Foreign bodies thrown at high speed by machining, grinding, or hammering are other causes of penetrating trauma.
CHEMICAL INJURY
- A chemical injury to the eye can be caused by a work-related accident. It can also be caused by common household products such as cleaning solutions, garden chemicals, solvents, or other types of chemicals. Fumes and aerosols can also cause chemical burns.
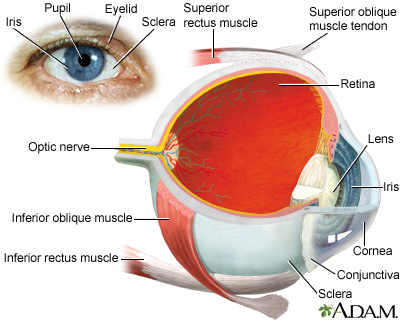
- The cornea is the clear (transparent) tissue covering the front of the eye.
- With acid burns, the haze on the cornea caused by the injury often clears and there is a good chance of recovery.
- Alkaline substances such as lime, lye, drain cleaners, and sodium hydroxide found in refrigeration equipment may cause permanent damage to the cornea.
- It is important to flush out the eye with large amounts of clean water or salt water (saline). This kind of injury needs medical care right away.
FOREIGN OBJECT IN THE EYE AND CORNEAL INJURIES
- The cornea is the clear (transparent) tissue covering the front of the eye.
- Dust, sand, and other debris can easily become embedded in the cornea without entering the eyeball. Persistent pain, sensitivity to light, and redness are signs that treatment is needed.
- An injury to the eyelid may be a sign of a severe injury to the eye itself.
Symptoms
Depending on the type of injury, any of the following symptoms may be present:
- Bleeding or other discharge from or around the eye
- Bruising
- Decreased vision
- Double vision
- Eye pain
- Headache
- Itchy eyes
- Loss of vision, total or partial, one eye or both
- Pupils of unequal size
- Redness -- bloodshot appearance
- Sensation of something in the eye
- Sensitivity to light
- Stinging or burning in the eye
First Aid
Take prompt action and follow the steps below if you or someone else have an eye injury. Always wash your hands with soap and water before touching the eye or eyelid.
SMALL FOREIGN OBJECT ON THE EYE OR EYELID
The eye will often clear itself of tiny objects, like eyelashes and sand, through blinking and tearing. If not, don't rub the eye or squeeze the eyelids. Here's how to examine someone else's eye:
- Examine the eye in a well-lighted area. Do not press on the eye.
- To find the object, have the person look up and down, then from side to side.
- If you cannot find the object, grasp the lower eyelid and gently pull it down to look under the lower eyelid. To look under the upper lid, ask the person to open both eyes and look down. Place a clean cotton swab on the outside of the upper lid. Grasp the eyelashes and gently fold the lid over the cotton swab.
- If the object is on an eyelid, try to gently flush it out with clean water. If that does not work, try touching a second cotton swab to the object to remove it.
- If the object is on the surface of the eye, try gently rinsing the eye with clean water. If available, use an eye dropper or a bottle of eye drops, such as artificial tears, positioned above the outer corner of the eye. Do not touch the eye itself with the dropper or bottle tip.
- A scratchy feeling or other minor discomfort may continue after removing eyelashes and other tiny objects. This should go away within a day or two. If discomfort or blurred vision continues, get medical help.
OBJECT STUCK OR EMBEDDED IN THE EYE
- Leave the object in place. Do not try to remove the object. Do not touch it or apply any pressure to it.
- Calm and reassure the person.
- Loosely bandage both eyes. Covering both eyes helps prevent eye movement. If the object is large, place a clean paper cup or something similar over the injured eye and tape it in place. This prevents the object from being pressed on, which can injure the eye further.
- Get medical help right away. Do not delay.
CHEMICAL IN THE EYE
- Flush with a gentle stream of cool tap water right away. Turn the person's head so the injured eye is down and to the side. Holding the eyelid open, allow running water from the faucet to flush the eye for 15 minutes.
- If both eyes are affected, or if the chemicals are also on other parts of the body, have the person take a shower.
- If the person is wearing contact lenses and the lenses did not flush out from the running water, have the person try to remove the contacts after the flushing.
- Keep flushing the eye with clean water or saline solution for at least 15 minutes.
- Seek medical help right away. Do not delay.
EYE CUT, SCRATCH, OR BLOW TO THE EYE
- Gently apply a clean cool compress to the eye to reduce swelling and help stop bleeding. Do not apply pressure to control bleeding.
- If blood is pooling in the eye, cover both eyes with a clean cloth or sterile dressing.
- Seek medical help right away. Do not delay.
EYELID CUTS
- Carefully wash the eyelid. If the cut is bleeding, apply gentle pressure with a clean, dry cloth until the bleeding stops. Do not press on the eyeball. The cut may go all the way through the eyelid, so there could also be a cut in the eyeball. It is usually safe to press on the bone around the eye.
- Cover with a clean dressing.
- Place a cool compress on the dressing to reduce pain and swelling.
- Seek medical help right away. Do not delay.
DO NOT
- Do not press or rub an injured eye.
- Do not remove contact lenses unless rapid swelling is occurring, there is a chemical injury and the contacts did not come out with the water flush, or you cannot get prompt medical help.
- Do not attempt to remove a foreign body or any object that appears to be embedded (stuck) in any part of the eye. Get medical help right away.
- Do not use cotton swabs, tweezers, or anything else on the colored part of the eye. Cotton swabs should only be used on the inside or outside of the eyelid or on the white of the eye.
When to Contact a Medical Professional
Seek emergency medical care if:
- There appears to be a scratch, cut, or something has gone into (penetrated) the eyeball.
- Any chemical gets into the eye.
- The eye is painful and red.
- Nausea or headache occur with the eye pain (this may be a symptom of glaucoma or stroke).
- There is any change in vision (such as blurred or double vision).
- There is uncontrollable bleeding.
Prevention
Supervise children carefully. Teach them how to be safe.
Always wear protective eye gear when:
- Using power tools, hammers, or other striking tools
- Working with toxic chemicals
- Cycling or when in windy and dusty areas
- Participating in sports that have a high likelihood of getting hit in the eye with a ball, such as indoor racket sports
Images
References
Dag Y, Aydin S, Kumantas E. The profile of patients attending to the general emergency department with ocular complaints within the last year: is it a true ocular emergency? BMC Ophthalmology. 2024;24(1):330. PMID: 39112942 pubmed.ncbi.nlm.nih.gov/39112942/.
Guluma K, Lee JE. Ophthalmology. In: Walls RM, ed. Rosen's Emergency Medicine: Concepts and Clinical Practice. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 57.
Muth CC. Eye emergencies. JAMA. 2017;318(7):676. jamanetwork.com/journals/jama/fullarticle/2648633. Updated August 15, 2017. Accessed May 9, 2025.
Vrcek I, Somogyi M, Reed D, Epstein A, Durairaj VD. Evaluation and management of periorbital soft tissue trauma. In: Yanoff M, Duker JS, eds. Ophthalmology. 6th ed. Philadelphia, PA: Elsevier; 2023:chap 12.9.
Review Date 4/29/2025
Updated by: Franklin W. Lusby, MD, Ophthalmologist, Lusby Vision Institute, La Jolla, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.