Acne is a skin condition that causes pimples or "zits." Whiteheads (closed comedones), blackheads (open comedones), red, inflamed papules, and nodules or cysts may develop. These most often occur on the face, neck, upper trunk and upper arms.
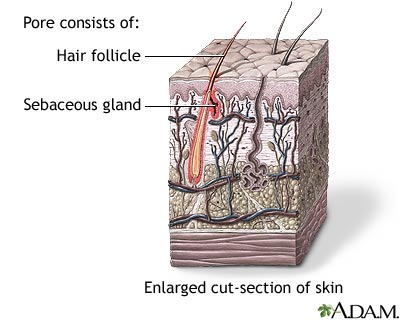
Acne occurs when tiny pores on the surface of the skin become clogged. The pores can become plugged by substances on the surface of the skin. More commonly they develop from a mixture of the natural oils of the skin and the dead cells shed from the inside of the pore. These plugs are called comedones. Acne is most common in teenagers. But anyone can get acne.
Acne breakouts can be triggered by:
- Hormonal changes
- Use of oily skin or hair care products
- Certain medicines
- Sweat
- Humidity
- Diet
Daily Skin Care
To keep your pores from clogging and your skin from becoming too oily:
- Clean your skin gently with a mild, non-drying soap.
- It may help to use a wash with salicylic acid or benzoyl peroxide if your skin is oily and prone to acne. Remove all dirt or make up.
- Wash once or twice a day, and also after exercising. Avoid scrubbing or repeated, frequent skin washing.
- Shampoo your hair daily, if it is oily.
- Comb or pull your hair back to keep the hair out of your face.
- Avoid using rubbing alcohol or toners that are very drying to the skin.
- Avoid oil-based cosmetics.
Acne medicines can cause skin drying or peeling. Use a moisturizer or skin cream that is water-based or "noncomedogenic" or that clearly states that is safe to use on the face and will not cause acne. Remember that products that say they are noncomedogenic might still cause acne in you personally. Therefore, avoid any product that you find makes your acne worse.
A small amount of sun exposure may improve acne slightly. However, too much exposure to sun or in tanning booths increases the risk for skin cancer. Some acne medicines can make your skin more sensitive to the sun. Use sunscreen and hats regularly if you are taking these medicines.
Minimizing dairy and high glycemic index foods may help decrease acne flares.
To further prevent acne:
- Do not aggressively squeeze, scratch, pick, or rub pimples. This can lead to skin infections as well as scarring and delayed healing.
- Avoid wearing tight headbands, baseball caps, and other hats.
- Avoid touching your face.
- Avoid greasy cosmetics or creams.
- Do not leave make up on overnight.
Acne Medicines
If daily skin care does not clear up blemishes, try over-the-counter acne medicines that you apply to your skin.
- These products may contain benzoyl peroxide, sulfur, adapalene, resorcinol, or salicylic acid.
- They work by killing bacteria, drying up skin oils, or causing the top layer of your skin to peel.
- They may cause redness or peeling of the skin.
If these acne medicines cause your skin to become irritated:
- Try using smaller amounts. A drop the size of a pea will cover the entire face.
- Use the medicines only every other or third day until your skin gets used to them.
- Wait 10 to 15 minutes after washing your face before applying these medicines.
Treatments From Your Health Care Provider
If pimples are still a problem after you've tried over-the-counter medicines, your health care provider may suggest:
- Antibiotics in the form of pills or creams that you put on your skin
- Prescription gels or creams containing a retinoid to help clear up the pimples
- Hormone pills for women whose acne is made worse by hormonal changes
- Isotretinoin pills for severe acne
- A light based procedure called photodynamic therapy
- Chemical peels
When to Call the Doctor
Contact your provider or your dermatologist if:
- Self-care steps and over-the-counter medicine do not help after several months.
- Your acne is painful (for example, you have a lot of redness around the pimples, or you have cysts).
- Your acne is getting worse.
- You develop scars as your acne clears up.
- Acne is causing emotional stress.
Alternative Names
Acne vulgaris - self-care; Cystic acne - self-care; Pimples - self-care; Zits - self-care
References
American Academy of Dermatology Association website. Can the right diet get rid of acne? www.aad.org/public/diseases/acne/causes/diet. Accessed March 4, 2026.
Draelos ZD. Cosmetics and cosmeceuticals. In: Bolognia JL, Schaffer JV, Cerroni L, eds. Dermatology. 5th ed. Philadelphia, PA: Elsevier; 2025:chap 153.
James WD. Acne. In: James WD, ed. Andrews' Diseases of the Skin: Clinical Dermatology. 14th ed. Philadelphia, PA: Elsevier; 2026:chap 11.
Paller AS, Mancini AJ. Acne vulgaris and other disorders of the sebaceous and sweat glands. In: Paller AS, Mancini AJ, eds. Paller and Mancini - Hurwitz Clinical Pediatric Dermatology. 6th ed. St Louis, MO: Elsevier; 2022:chap 8.
Zaenglein AL, Nelson AM, Lalor LEB. Acne vulgaris. In: Bolognia JL, Schaffer JV, Cerroni L, eds. Dermatology. 5th ed. Philadelphia, PA: Elsevier; 2025:chap 36.
Review Date 1/28/2026
Updated by: Ramin Fathi, MD, FAAD, Director, Phoenix Surgical Dermatology Group, Phoenix, AZ. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.