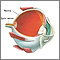
Laser photocoagulation is eye surgery using a laser to shrink or destroy abnormal structures in the retina, or to intentionally cause scarring that can help certain eye conditions.
Description
Your eye doctor will perform this surgery at an outpatient or office setting.
Photocoagulation takes place by using the laser to create a microscopic burn in the target tissue. The laser spots are usually applied in 1 of 3 patterns.
Before the procedure, you will be given eye drops to dilate your pupils. Rarely, you will get a shot of a local anesthetic. The shot may be uncomfortable. You will be awake and pain-free during the procedure.
- You will be seated with your chin in a chin rest. A special lens will be placed on your eye. The lens contains mirrors that help the doctor aim the laser. You will be instructed to look straight ahead or at a target light with your other eye.
- The doctor will aim the laser at the area of the retina needing treatment. With each pulse of the laser, you will see a flash of light. Depending on the condition being treated, there may be only a few pulses, or as many as 500.
Why the Procedure is Performed
Diabetes can harm the eyes by causing diabetic retinopathy. It is one of the most common eye diseases that needs laser photocoagulation. It can damage the retina, the back part of your eye. The most severe form of the condition is proliferative diabetic retinopathy, in which abnormal vessels grow on the retina. Over time, these vessels can bleed or cause scarring of the retina.
In laser photocoagulation for diabetic retinopathy, laser energy is aimed at certain areas of the retina to prevent abnormal vessels from growing or shrinking those that may already be there. Sometimes it is done to make edema fluid in the center of the retina (macula) go away.
This surgery may also be used to treat the following eye problems:
- Retinal tumor
- Macular degeneration, an eye disorder that slowly destroys sharp, central vision
- A tear in the retina
- A blockage of the small veins that carry blood away from the retina
- Retinal detachment, when the retina in the back of the eye separates from the layers below
Risks
Since each pulse of the laser causes a microscopic burn in the retina, you may develop:
- Mild loss of vision
- Reduced night vision
- Blind spots
- Reduced side vision
- Difficulty focusing
- Blurred vision
- Reduced color vision
If not treated, diabetic retinopathy can cause permanent blindness.
Before the Procedure
Special preparations are rarely needed before laser photocoagulation. Usually, both eyes will be dilated for the procedure.
Arrange to have someone to drive you home after the procedure.
After the Procedure
You vision will be blurry for the first 24 hours. You may see floaters, but these will subside over time. If your treatment was for macular edema, your vision may seem worse for a few days.
Outlook (Prognosis)
Laser surgery works best in the early stages of vision loss. It cannot bring back lost vision. However, it can greatly reduce the risk for permanent vision loss.
Managing your diabetes can help prevent diabetic retinopathy. Follow your eye doctor's advice on how to protect your vision. Have eye exams as often as recommended, usually once every 1 to 2 years.
Alternative Names
Laser coagulation; Laser eye surgery; Photocoagulation; Laser photocoagulation - diabetic eye disease; Laser photocoagulation - diabetic retinopathy; Focal photocoagulation; Scatter (or pan retinal) photocoagulation; Proliferative retinopathy - laser; PRP - laser; Grid pattern photocoagulation - laser
Images
References
American Academy of Ophthalmology website. Diabetic macular edema: diagnosis and management. www.aao.org/eyenet/article/diabetic-macular-edema-diagnosis-and-management. Updated May 2021. Accessed February 4, 2026.
Lim JI, Kim SJ, Bailey ST, et al. Diabetic retinopathy Preferred Practice Pattern®. Ophthalmology. 2025;132(4):P75-P162. PMID: 39918521 pubmed.ncbi.nlm.nih.gov/39918521/.
Silva PS, Salongcay RP. Diabetic retinopathy. In: Yanoff M, Duker JS, eds. Ophthalmology. 6th ed. Philadelphia, PA: Elsevier; 2023:chap 6.18.
Wiley HE, Chew EY, Ferris FL. Nonproliferative diabetic retinopathy and diabetic macular edema. In: Sadda SR, Sarraf D, Freund KB, et al, eds. Ryan's Retina. 7th ed. Philadelphia, PA: Elsevier; 2023:chap 49.
Review Date 1/27/2026
Updated by: Franklin W. Lusby, MD, Ophthalmologist, Lusby Vision Institute, La Jolla, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.