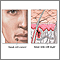
Mohs micrographic surgery is a way to treat and cure certain skin cancers. Surgeons trained in the Mohs procedure can do this surgery. It allows skin cancer to be removed with less damage to the healthy skin around it.
Description
Mohs surgery usually takes place in the surgeon's office. The surgery is usually started early in the morning and is done in one day. Sometimes if the tumor is big or you need reconstruction, it may take two visits.
During the procedure, the surgeon removes the cancer in layers until all the cancer has been removed. The surgeon will:
- Numb your skin where cancer is so you do not feel any pain. You stay awake for the procedure.
- Remove the visible tumor along with a thin layer of tissue next to the tumor.
- Look at the tissue under a microscope.
- Check for cancer. If there is still cancer in that layer, the surgeon will take out another layer and look at that under the microscope.
- Keep repeating this procedure until there is no cancer found in a layer. Each round takes about 1 hour. The surgery takes 10 to 20 minutes, while preparing the tissue and looking at it under the microscope takes 40 to 50 minutes.
- Do 2 or more rounds to get all of the cancer. Larger or deep tumors may need more layers.
- Apply a pressure dressing to the wound between layers.
- Close the wound with stitches after the skin cancer is removed completely. Small wounds sometimes do not require stitches. Larger wounds may require a skin graft or skin flap to close the wound.
Why the Procedure is Performed
Mohs surgery can be used for most skin cancers, such as basal cell or squamous cell skin cancers.
Mohs surgery may be preferred when the skin cancer is on an area where:
- It is important to remove as little tissue as possible, such as the scalp, face, neck, hands, feet, nails, shins, or genitalia.
- There is a scar or prior radiation treatment was used.
- There is a higher chance the tumor will come back, such as on the ears, lips, nose, eyelids, temples, hands, feet, nails, or genitalia.
Mohs surgery may also be preferred when:
- The skin cancer was already treated, and it was not completely removed, or it came back.
- The skin cancer is large, or the edges of the skin cancer are not clear.
- Your immune system is not working well due to cancer, cancer treatments, or medicines you are taking.
- The tumor is deeper.
Risks
Mohs surgery is generally safe. With Mohs surgery, you do not need to be put asleep (general anesthesia) as you would with other surgeries.
While rare, these are some risks for this surgery:
- Infection.
- Nerve damage that causes numbness or a burning sensation. This usually goes away.
- Larger scars that are raised and red, called keloids.
- Bleeding.
Before the Procedure
Your surgeon will explain what you should do to prepare for your surgery. You may be asked to:
- Stop taking certain medicines, such as aspirin or other blood thinners that are not medically indicated. Do not stop taking any prescription medicines unless your surgeon tells you to stop.
- Stop smoking.
- Arrange to have someone take you home after your surgery if needed.
After the Procedure
Taking proper care of your wound after surgery will help your skin look its best. Your surgeon will talk with you about your options:
- Let a small wound heal itself. Most small wounds heal well on their own.
- Use stitches to close the wound.
- Use skin grafts. The surgeon covers the wound using skin from another part of your body.
- Use skin flaps. The surgeon covers the wound with the skin next to your wound. Skin near your wound matches in color and texture.
Outlook (Prognosis)
Mohs surgery has a 99% cure rate in treating skin cancer.
With this surgery, the smallest amount of tissue possible is removed. You will have a smaller scar than you might have with other treatment options.
Alternative Names
Skin cancer - Mohs surgery; Basal cell skin cancer - Mohs surgery; Squamous cell skin cancer - Mohs surgery; Melanoma - Mohs surgery
Images
References
American College of Mohs Surgery website. The Mohs step-by-step process. www.mohscollege.org/for-patients/about-mohs-surgery/the-mohs-step-by-step-process. Accessed November 8, 2024.
Lam C, Vidimos AT. Mohs micrographic surgery. In: Bolognia JL, Schaffer JV, Cerroni L, eds. Dermatology. 4th ed. Philadelphia, PA: Elsevier; 2018:chap 150.
Review Date 10/14/2024
Updated by: Elika Hoss, MD, Assistant Professor of Dermatology, Mayo Clinic, Scottsdale, AZ. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.