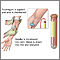
A1C is a lab test that shows the average level of blood sugar (glucose) over the previous 3 months. It shows how well you are controlling your blood sugar to help prevent complications from diabetes.
How the Test is Performed
A blood sample is needed. Two methods are available:
- Blood drawn from a vein. This is done at a lab.
- Finger stick. This can be done in your health care provider's office. Or, you may be prescribed a kit that you can use at home. Results by finger stick may differ slightly from blood drawn from a vein, but in most cases can also be used to monitor your treatment.
How to Prepare for the Test
No special preparation is needed. The food you have recently eaten does not affect the A1C test, so you do not need to fast to prepare for this blood test.
How the Test will Feel
With a finger stick, you may feel slight pain.
With blood drawn from a vein, you may feel a slight pinch or some stinging when the needle is inserted. Afterward, there may be some throbbing or a slight bruise. This soon goes away.
Why the Test is Performed
Your provider may order this test if you have diabetes. It shows how well you are controlling your diabetes.
The test may also be used to screen for diabetes.
Ask your provider how often you should have your A1C level tested. Usually, for people with diabetes, testing every 3 or 6 months is recommended.
Normal Results
The following are the results when A1C is being used to diagnose diabetes:
- Normal (no diabetes): Less than 5.7%
- Pre-diabetes: 5.7% to 6.4%
- Diabetes: 6.5% or higher
If you have diabetes, you and your provider will discuss the ideal range for you, which may vary based on your age. For many people, the goal is to keep the level below 7%.
The test result may be incorrect in people with anemia, kidney disease, liver disease, or certain blood disorders (thalassemia), or after a blood transfusion. Talk to your provider if you have any of these conditions. Certain medicines can also result in a false A1C level.
The examples above are common measurements for results of these tests. Normal value ranges may vary slightly among different laboratories. Talk to your provider about the meaning of your specific test results.
What Abnormal Results Mean
An abnormal result means that you have had a high blood sugar level over a period of weeks to months.
If your A1C is 6.5% or higher and you do not already have diabetes, you may be diagnosed with diabetes.
If your level is above 7% and you have diabetes, it often means that your blood sugar is not as well controlled as would be ideal. You and your provider should determine your target A1C.
Many labs now use the A1C to calculate an estimated average glucose (eAG). This estimate may be different from the average blood sugars you are recording from your glucose meter or continuous glucose monitor. Talk to your provider about what this means. The actual blood sugar readings are usually more reliable than the estimated average glucose based on the A1C.
The higher your A1C, the higher the risk that you will develop problems such as:
If your A1C stays high, talk to your provider about how best to manage your blood sugar.
Risks
There is little risk involved with having your blood taken. Veins and arteries vary in size from one person to another and from one side of the body to the other. Taking blood from some people may be more difficult than from others.
Other risks of having blood drawn are slight, but may include:
- Excessive bleeding
- Multiple punctures to locate veins
- Fainting or feeling lightheaded
- Hematoma (blood accumulating under the skin)
- Infection (a slight risk any time the skin is broken)
Alternative Names
HbA1C test; Glycated hemoglobin test; Glycohemoglobin test; Hemoglobin A1C; Diabetes - A1C; Diabetic - A1C
Patient Instructions
Images
References
American Diabetes Association Professional Practice Committee. 6. Glycemic Goals and Hypoglycemia: Standards of Care in Diabetes-2024. Diabetes Care. 2024;47(Suppl 1):S111-S125. PMID: 38078586 pubmed.ncbi.nlm.nih.gov/38078586/.
Chernecky CC, Berger BJ. Glycosylated hemoglobin (GHb, glycohemoglobin, glycated hemoglobin, HbA1a, HbA1b, HbA1c) - blood. In: Chernecky CC, Berger BJ, eds. Laboratory Tests and Diagnostic Procedures. 6th ed. St Louis, MO: Elsevier Saunders; 2013:596-597.
Dhatariya KK, Umpierrez GE, Crandall JP. Diabetes. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 210.
Maloney GE, Glauser JM. Diabetes mellitus and disorders of glucose homeostasis In: Walls RM, ed. Rosen's Emergency Medicine: Concepts and Clinical Practice. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 115.
Review Date 5/20/2024
Updated by: Sandeep K. Dhaliwal, MD, board-certified in Diabetes, Endocrinology, and Metabolism, Springfield, VA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.