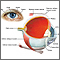
Tonometry is a test to measure the pressure inside your eyes. The test is used to screen for glaucoma. It is also used to measure how well glaucoma treatment is working.
How the Test is Performed
There are three main methods of measuring eye pressure.
The most accurate method measures the force needed to flatten an area of the cornea.
- The surface of the eye is numbed with eye drops. A fine strip of paper stained with orange dye is held to the side of the eye. The dye stains the front of the eye to help with the exam. Sometimes the dye is in the numbing drops.
- You will rest your chin and forehead on the support of a slit lamp so that your head is steady. You will be asked to keep your eyes open and to look straight ahead. The lamp is moved forward until the tip of the tonometer just touches the cornea.
- Blue light is used so that the orange dye will glow green. The health care provider looks through the eyepiece on the slit-lamp and adjusts a dial on the machine to give the pressure reading.
- There is no discomfort with the test.
A second method uses a handheld device shaped like a pen. You are given numbing eye drops to prevent any discomfort. The device touches the surface of the cornea and instantly records eye pressure.
The last method is the noncontact method (air puff). In this method, your chin rests on a device similar to a slit lamp.
- You stare straight into the examining device. When you are at the correct distance from the device, a tiny beam of light reflects off of your cornea onto a detector.
- When the test is performed, a puff of air will slightly flatten the cornea; how much it flattens depends on the eye pressure.
- This causes the tiny beam of light to move to a different spot on the detector. The instrument calculates eye pressure by looking at how far the beam of light moved.
How to Prepare for the Test
Remove contact lenses before the exam. The dye can permanently stain contact lenses.
Tell your provider if you have a history of corneal ulcers or eye infections, or a history of glaucoma in your family. Always tell your provider what medicines you are taking.
How the Test will Feel
If numbing eye drops were used, you should not have any pain. In the noncontact method, you may feel mild pressure on your eye for a brief moment from the air puff.
Why the Test is Performed
Tonometry is a test to measure the pressure inside your eyes. The test is used to screen for glaucoma and to measure how well glaucoma treatment is working.
People over age 40 years, particularly African Americans, have the highest risk for developing glaucoma. Regular eye exams can help detect glaucoma early. If it is detected early, glaucoma can be treated before too much damage is done.
The test may also be done before and after eye surgery.
Normal Results
A normal result means your eye pressure is within the normal range. The normal eye pressure range is 10 to 21 mm Hg.
The thickness of your cornea can affect measurements. Normal eyes with thick corneas have higher readings, and normal eyes with thin corneas have lower readings. A thin cornea with a high reading may be very abnormal (the actual eye pressure will be higher than shown on the tonometer).
A corneal thickness measurement (pachymetry) is needed to get a correct pressure measurement.
Talk to your provider about the meaning of your specific test results.
What Abnormal Results Mean
Abnormal results may be due to:
- Glaucoma
- Hyphema (blood in the front chamber of the eye)
- Inflammation in the eye
- Injury to the eye or head
- Recent eye surgery
Risks
If the applanation method is used, there is a small chance the cornea may be scratched (corneal abrasion). The scratch will normally heal within a few days.
Alternative Names
Intraocular pressure (IOP) measurement; Glaucoma test; Goldmann applanation tonometry (GAT)
Images
References
Chen S, Lee BD, Al-Aswad LA. Clinical examination of glaucoma. In: Yanoff M, Duker JS, eds. Ophthalmology. 6th ed. Philadelphia, PA: Elsevier; 2023:chap 10.4.
Knoop KJ, Dennis WR. Ophthalmologic procedures. In: Roberts JR, Custalow CB, Thomsen TW, eds. Roberts and Hedges' Clinical Procedures in Emergency Medicine and Acute Care. 7th ed. Philadelphia, PA: Elsevier; 2019:chap 62.
Quérat L, Chen E. Impact of self-tonometry on glaucoma treatment decision. Acta Ophthalmol. 2023;101(2):e246-e251. PMID: 36147012 pubmed.ncbi.nlm.nih.gov/36147012/.
Review Date 8/5/2024
Updated by: Franklin W. Lusby, MD, Ophthalmologist, Lusby Vision Institute, La Jolla, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.