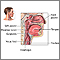
A stuffy or congested nose occurs when the tissues lining the nose become swollen. The swelling is due to inflamed blood vessels.
The problem may also include nasal discharge or runny nose. If excess mucus runs down the back of the throat (postnasal drip), it may cause a cough or sore throat.
Considerations
Most of the time, nasal congestion in older children and adolescents is not serious by itself, but can cause other problems.
When nasal stuffiness is just on one side, the child may have inserted something into their nose.
Nasal congestion can interfere with the ears, hearing, and speech development. Congestion that is very bad may interfere with sleep.
The mucous drainage may plug up the eustachian tube between the nose and the ear, causing an ear infection and pain. The mucous drip may also plug the sinus passages, causing a sinus infection and pain.
Causes
A stuffy or runny nose may be caused by:
- Common cold
- Flu
- Sinus infection
The congestion typically goes away by itself within a week.
Congestion also can be caused by:
- Hay fever or other allergies
- Use of some nasal sprays or drops bought without a prescription for more than 3 days (may make nasal stuffiness worse)
- Nasal polyps, sac-like growths of inflamed tissue lining the nose or sinuses
- Pregnancy
- Vasomotor rhinitis
- Small objects in the nostril
Home Care
Tips to help infants and younger children include:
- Raise the head of your child's bed. Put a pillow underneath the head of the mattress. Or, place books or boards under the legs at the head of the bed.
- Older children may drink extra fluids, but those fluids should be sugar-free.
- You can try a cool-mist vaporizer, but avoid putting too much moisture in the room. Clean the vaporizer every day with bleach or a disinfectant cleaning product.
- You can also steam up the bathroom shower and bring your child in there before bed.
A nasal wash can help remove mucus from your child's nose.
- You can buy a saline spray at a drugstore or make one at home. To make one, use 1 cup (240 milliliters) of warm water, 1/2 teaspoon (3 grams) of salt, and a pinch of baking soda.
- Use gentle saline nasal sprays 3 to 4 times per day.
If your child has allergies:
- Your health care provider may also prescribe nasal sprays that treat allergy symptoms.
- Learn how to avoid triggers that make allergies worse.
Nasal sprays are not recommended for children under age 2. Don't use over-the-counter nasal sprays more often than 3 days on and 3 days off, unless told to by your provider.
You can buy cough and cold medicines without a prescription. They do not seem to be effective in children.
When to Contact a Medical Professional
Contact your child's provider if your child has any of the following:
- A stuffy nose with swelling of the forehead, eyes, side of the nose, or cheek, or that occurs with blurred vision
- More throat pain, or white or yellow spots on the tonsils or other parts of the throat
- Discharge from the nose that has a bad smell, comes from only one side, or is a color other than white or yellow
- Cough that lasts longer than 10 days, or produces yellow-green or gray mucus
- Symptoms that last more than 3 weeks
- Nasal discharge with fever
What to Expect at Your Office Visit
Your child's provider may perform a physical exam that focuses on the ears, nose, throat, and airways.
Tests that may be done include:
- Allergy tests on skin and blood tests
- Blood tests (such as CBC or blood differential)
- Sputum culture and throat culture
- X-rays of the sinuses and chest x-ray
- CT scan of the head
Alternative Names
Nose - congested; Congested nose; Runny nose; Postnasal drip; Rhinorrhea
Images
References
McGann KA, Long SS. Respiratory tract symptom complexes. In: Long SS, ed. Principles and Practice of Pediatric Infectious Diseases. 6th ed. Philadelphia, PA: Elsevier; 2023:chap 21.
Perry TT, Sicherer SH. Allergic rhinitis. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 184.
Richardson KM, Schuster JE. The common cold. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 428.
Review Date 7/3/2025
Updated by: Linda J. Vorvick, MD, Clinical Professor Emeritus, Department of Family Medicine, UW Medicine, School of Medicine, University of Washington, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.