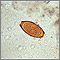
Whipworm infection is an infection of the large intestine with a type of roundworm.
Causes
Whipworm infection is caused by the roundworm Trichuris trichiura. It is a common infection that mainly affects children.
Children may become infected if they swallow soil contaminated with whipworm eggs. When the eggs hatch inside the body, the whipworm sticks inside the wall of the large intestine.
Whipworm is found throughout the world, especially in countries with warm, humid climates. Some outbreaks have been traced to contaminated vegetables (caused by soil contamination).
Symptoms
Most people who have whipworm infections don't have symptoms. Symptoms mainly occur in children, and range from mild to severe. A severe infection may cause:
- Bloody diarrhea
- Iron-deficiency anemia
- Fecal incontinence (during sleep)
- Rectal prolapse (the rectum comes out of the anus)
Exams and Tests
A stool ova and parasites exam reveals the presence of whipworm eggs.
Treatment
The medicine albendazole is commonly prescribed when the infection causes symptoms. A different anti-worm medicine may also be prescribed.
Outlook (Prognosis)
Full recovery is expected with treatment.
When to Contact a Medical Professional
Seek medical attention if you or your child develop bloody diarrhea. In addition to whipworm, many other infections and illnesses can cause similar symptoms.
Prevention
Improved facilities for feces disposal have decreased the incidence of whipworm.
Always wash your hands before handling food. Teach your children to wash their hands, too. Thoroughly washing food may also help prevent this condition.
Alternative Names
Intestinal parasite - whipworm; Trichuriasis; Round worm - trichuriasis
Images
References
Diemert DJ. Nematode infections. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 327.
Dobbs KR, Dent AE. Trichuriasis (Trichuris trichiura). In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 339.
Mejia R, Weatherhead J, Hotez PJ. Intestinal nematodes (roundworms). In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 286.
Review Date 11/10/2024
Updated by: Jatin M. Vyas, MD, PhD, Roy and Diana Vagelos Professor in Medicine, Columbia University Vagelos College of Physicians and Surgeons, Division of Infectious Diseases, Department of Medicine, New York, NY. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.