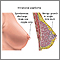
Intraductal papilloma is a small, noncancerous (benign) tumor that grows in a milk duct of the breast.
Causes
Intraductal papilloma occurs most often in women ages 35 to 55. The causes and risk factors are unknown.
Symptoms
Symptoms include:
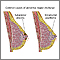
- Breast lump, which could be near the nipple
- Nipple discharge, which may be clear or bloodstained
These findings may be in just one breast or in both breasts. Usually, there is a single intraductal papilloma. In some cases there may be multiple intraductal papillomas.
For the most part, these papillomas do not cause pain.
Exams and Tests
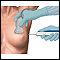
Your health care provider might feel a small lump under the nipple, but this lump cannot always be felt. There may be discharge from the nipple. Sometimes, an intraductal papilloma is found on a mammogram or ultrasound, and then diagnosed by a needle biopsy.
If there is a mass or nipple discharge, both a mammogram and an ultrasound should be performed.
A breast MRI is sometimes recommended.
An intraductal papilloma is diagnosed on needle biopsy or surgical biopsy.
Treatment
If a needle biopsy shows an intraductal papilloma, the papilloma may be removed with surgery, or watched over time with exams and imaging.
Outlook (Prognosis)
For the most part, intraductal papillomas do not appear to increase the risk of developing breast cancer.
The outcome is excellent for people with one papilloma. The risk for cancer may be higher for:
- Women with multiple papillomas
- Women who get them at an early age
- Women with a family history of cancer
- Women who have abnormal cells in the biopsy
Possible Complications
Complications of surgery can include bleeding, infection, scarring, and anesthesia risks. If the biopsy shows cancer, you may need further surgery and treatment.
When to Contact a Medical Professional
Contact your provider if you notice any breast discharge or a breast lump.
Prevention
There is no known way to prevent intraductal papilloma. Breast self-exams and screening mammograms can help detect the disease early.
References
Cox DM, Lippe C, Geletzke AK, et al. Etiology and management of benign breast disease. In: Klimberg VS, Gradishar WJ, Bland KI, Korourian S, White J, Copeland EM, eds. Bland and Copeland's The Breast: Comprehensive Management of Benign and Malignant Disorders. 6th ed. Philadelphia, PA: Elsevier; 2024:chap 14.
Davidson NE. Breast cancer and benign breast disorders. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 183.
Weiser R, Klimberg VS, Hunt KK. Diseases of the breast. In: Tyler DS, Hayes-Dixon A, Hines OJ, et al, eds. Sabiston Textbook of Surgery. 22nd ed. Philadelphia, PA: Elsevier; 2026:chap 68.
Review Date 10/7/2025
Updated by: John Meilahn, MD, General Surgeon, Wyndmoor, PA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.