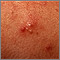
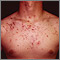
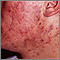
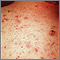
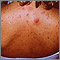
Acne is a skin condition that causes pimples or "zits." Whiteheads, blackheads, and red, inflamed bumps or patches of skin (such as cysts) may develop.
Causes
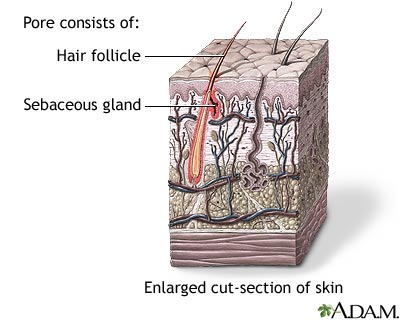
Acne occurs when tiny holes on the surface of the skin become clogged. These holes are called pores.
- Each pore opens to a follicle. A follicle contains a hair and an oil gland. The oil released by the gland helps remove old skin cells and keeps your skin soft.
- The glands can become blocked with a mixture of oil and skin cells. The blockage is called a plug or comedone. If the top of the plug is white, it is called a whitehead. It is called a blackhead if the top of the plug is dark.
- If bacteria become trapped in the plug, the body's immune system may react to it, causing pimples.
- Acne that is deep in your skin can cause hard, painful cysts. This is called nodulocystic acne.
Acne is most common in teenagers, but anyone can get acne, even babies. The problem tends to run in families.
Some things that may trigger acne include:
- Hormonal changes that make the skin oilier. These may be related to puberty, menstrual periods, pregnancy, birth control pills, or stress.
- Greasy or oily cosmetic and hair products.
- Certain medicines (such as steroids, testosterone, estrogen, and phenytoin). Birth control devices, such as some medicine-containing IUDs, can make acne worse.
- Heavy sweating and humidity.
- Excessively touching, resting on, or rubbing the skin.
Research does not show that chocolate, nuts, and greasy foods cause acne. Diets high in refined sugars or dairy products may be related to acne in some people, but this connection is controversial.
Symptoms
Acne commonly appears on the face and shoulders. It may also occur on the trunk, arms, legs, and buttocks. Skin changes include:
- Crusting of skin bumps
- Cysts
- Papules (small red bumps)
- Pustules (small red bumps containing white or yellow pus)
- Redness around the skin eruptions
- Scarring of the skin
- Whiteheads
- Blackheads
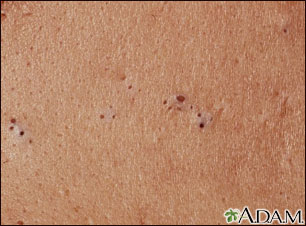
Exams and Tests
Your health care provider can diagnose acne by looking at your skin. Testing is not needed in most cases. Bacterial culture may be performed with certain patterns of acne or to check for infection if large pus bumps persist.
Treatment
SELF-CARE
Steps you can take to help your acne:
- Clean your skin gently with a mild, nondrying soap (such as Dove, Neutrogena, Cetaphil, CeraVe, or Basics).
- Look for water-based or noncomedogenic formulas for cosmetics and skin creams. (Noncomedogenic products have been tested and proven not to clog pores and cause acne in most people.)
- Remove all dirt or make-up. Wash once or twice a day, including after exercising.
- Avoid scrubbing or repeated skin washing.
- Shampoo your hair daily, especially if it is oily.
- Comb or pull your hair back to keep the hair out of your face.
What not to do:
- Try not to aggressively squeeze, scratch, pick, or rub the pimples. This can lead to skin infections, slower healing, and scarring.
- Avoid wearing tight headbands, baseball caps, and other hats.
- Avoid touching your face with your hands or fingers.
- Avoid greasy cosmetics or creams.
- Do not leave make-up on overnight.
If these steps do not clear up the blemishes, try over-the-counter acne medicines that you apply to your skin. Follow the directions carefully and apply these products sparingly.
- These products may contain benzoyl peroxide, sulfur, resorcinol, adapalene, or salicylic acid.
- They work by killing bacteria, drying up skin oils, or causing the top layer of your skin to peel.
- They may cause redness, drying, or excessive peeling of the skin.
- Be aware that benzoyl peroxide containing preparations can bleach or discolor towels and clothing.
A small amount of sun exposure may improve acne slightly, but tanning mostly hides the acne. Too much exposure to sunlight or ultraviolet rays is not recommended because it increases the risk for wrinkles and skin cancer.
MEDICINES FROM YOUR PROVIDER
If pimples are still a problem, your provider can prescribe stronger medicines and discuss other options with you.
Antibiotics may help some people with acne:
- Oral antibiotics (taken by mouth) such as tetracycline, doxycycline, minocycline, erythromycin, trimethoprim-sulfamethoxazole, and amoxicillin
- Topical antibiotics (applied to the skin) such as clindamycin, erythromycin, or dapsone
Creams or gels applied to the skin may be prescribed:
- Derivatives of vitamin A such as retinoic acid cream or gel (tretinoin, tazarotene)
- Prescription formulas of benzoyl peroxide, sulfur, resorcinol, or salicylic acid
- Topical azelaic acid
For women whose acne is caused or made worse by hormones:
- A pill called spironolactone may help.
- Birth control pills may help in some cases, though they may make acne worse in some women.
Minor procedures or treatments may also be helpful:
- Photodynamic therapy may be used. This is a treatment where a chemical that is activated by blue light is applied to the skin, followed by exposure to the light.
- Your provider may also suggest chemical skin peeling; removal of scars by dermabrasion; or removal, drainage, or injection of cysts with cortisone.
People who have cystic acne and scarring may try a medicine called isotretinoin. You will be watched closely when taking this medicine because of its side effects.
Pregnant women should not take isotretinoin, because it causes severe birth defects.
- Women taking isotretinoin must use 2 forms of birth control before starting the medicine and enroll in the iPledge program.
- Men also need to be enrolled in the iPledge program.
- Your provider will follow you on this medicine and you will have regular blood tests.
Outlook (Prognosis)
Most of the time, acne goes away after the teenage years, but it may last into middle age. The condition often responds well to treatment, but responses may take 6 to 8 weeks, and acne may flare up from time to time.
Scarring may occur if severe acne is not treated. Some people become very depressed if acne is not treated.
When to Contact a Medical Professional
Contact your provider if:
- Self-care steps and over-the-counter medicine do not help after several months.
- Your acne is very bad (for example, you have a lot of redness around the pimples, or you have cysts).
- Your acne is getting worse.
- You develop scars as your acne clears up.
- Acne is causing emotional stress.
If your baby has acne, contact the baby's provider if acne does not clear up on its own within 3 months.
Alternative Names
Acne vulgaris; Cystic acne; Pimples; Zits
References
Dinulos JGH. Acne, rosacea, and related disorders. In: Dinulos JGH, ed. Habif's Clinical Dermatology. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 7.
James WD. Acne. In: James WD, ed. Andrews' Diseases of the Skin: Clinical Dermatology. 14th ed. Philadelphia, PA: Elsevier; 2026:chap 11.
Lalor L. Acne. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 710.
Moon M, Guerrero AM, Li X, Koch E, Gehris RP. Dermatology. In: Zitelli BJ, McIntire SC, Nowalk AJ, Garrison J, eds. Zitelli and Davis' Atlas of Pediatric Physical Diagnosis. 8th ed. Philadelphia, PA: Elsevier; 2023:chap 8.
Review Date 8/2/2025
Updated by: Ramin Fathi, MD, FAAD, Director, Phoenix Surgical Dermatology Group, Phoenix, AZ. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.