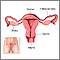
Birth control pills (BCPs) contain man-made forms of 2 hormones called estrogen and progestin. These hormones are made naturally in a woman's ovaries. BCPs can contain both of these hormones, or have progestin only.
Both hormones prevent a woman's ovary from releasing an egg during her menstrual cycle (called ovulation). They do this by changing the levels of the natural hormones the body makes.
Progestins also make the mucus around a woman's cervix thick and sticky. This helps prevent sperm from entering the uterus.
Information
BCPs are also called oral contraceptives or just "the pill." A health care provider must prescribe most types of BCPs but one was recently approved by the US Food and Drug Administration for over-the-counter use.
- The most common type of BCP combines the hormones estrogen and progestin. There are many different forms of this type of pill.
- The "mini-pill" is a type of BCP that contains only progestin, no estrogen. These pills are an option for women who do not like the side effects of estrogen or who cannot take estrogen for medical reasons.
- They can also be used after delivery in women who are breastfeeding.
All women who take BCPs need a check-up at least once a year. Women should also have their blood pressure checked 3 months after they begin to take the pill.
BCPs only work well if the woman remembers to take her pill daily without missing a day. Only 2 or 3 women out of 100 who take BCPs correctly for a year will get pregnant.
BCPs may cause many side effects. These include:
- Changes in menstrual cycles, no menstrual cycles, extra bleeding
- Nausea, mood changes, worsening of migraines (mostly due to estrogens)
- Breast tenderness and weight gain
Rare but dangerous risks from taking BCPs include:
- Blood clots
- Heart attack
- High blood pressure
- Stroke
BCPs without estrogen are much less likely to cause these problems. The risk is higher for women who smoke or have a history of high blood pressure, clotting disorders, or unhealthy cholesterol levels. However, the risks of developing these complications are much lower with either type of pill than with pregnancy.
Regular menstrual cycles will return within 3 to 6 months after a woman stops using most hormonal birth control methods.
Alternative Names
Contraception - pills - hormonal methods; Hormonal birth control methods; Birth control pills; Contraceptive pills; BCP; OCP; Family planning - BCP; Estrogen - BCP; Progestin - BCP
References
Allen RH, Huguenin A, Hickey M, Kaunitz AM. Hormonal contraception. In: Melmed S, Auchus RJ, Goldfine AB, Rosen CJ, Kopp PA, eds. Williams Textbook of Endocrinology. 15th ed. Philadelphia, PA: Elsevier; 2025:chap 16.
American College of Obstetricians and Gynecologists website. ACOG Practice Bulletin No. 206: Use of hormonal contraception in women with coexisting medical conditions. Obstet Gynecol. 2019;133(6):1288. Erratum for: Obstet Gynecol. 2019;133(2):e128-e150. PMID: 31135757 pubmed.ncbi.nlm.nih.gov/31135757/.
Harper DM, Wilfling LE, Blanner CF. Contraception. In: Rakel RE, Rakel DP, eds. Textbook of Family Medicine. 9th ed. Philadelphia, PA: Elsevier Saunders; 2016:chap 26.
Rivlin K, Davis AR. Contraception and abortion. In: Gershenson DM, Lentz GM, Valea FA, Lobo RA, eds. Comprehensive Gynecology. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 13.
Winikoff B, Grossman D. Contraception. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 220.
Review Date 3/31/2024
Updated by: LaQuita Martinez, MD, Department of Obstetrics and Gynecology, Emory Johns Creek Hospital, Alpharetta, GA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.