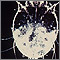
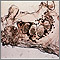
Scabies is an easily-spread skin disease caused by a very small mite.
Causes
Scabies is found among people of all groups and ages around the world.
- Scabies spread by skin-to-skin contact with another person who has scabies.
- Scabies is easily spread among people who are in close contact. Whole families are often affected.
Outbreaks of scabies are more common in nursing homes, nursing facilities, college dorms, and child care centers.
The mites that cause scabies burrow into the skin and lay their eggs. This forms a burrow that looks like a pencil mark. Eggs hatch in 21 days. The itchy rash is an allergic response to the mite.
Pets and animals usually do not spread human scabies. It is also very unlikely for scabies to be spread through swimming pools. It is difficult to spread scabies through clothing or bed linen.
A type of scabies called crusted (Norwegian) scabies is a severe infestation with very large numbers of mites. People whose immune systems are weakened are most affected.
Symptoms
Symptoms of scabies include:
- Severe itching, most often at night.
- Rashes, often between the fingers and toes, undersides of the wrists, armpits, women's breasts, and buttocks.
- Sores on the skin from scratching and digging.
- Thin lines (burrow marks) on the skin.
- Babies will likely have a rash all over the body, especially on the head, face, and neck, with sores on the palms and soles.
Scabies doesn't affect the face except in babies and in people with crusted scabies.
Exams and Tests
Your health care provider will examine your skin for signs of scabies.
Tests that may be done include:
- Scraping the skin burrows to remove mites, eggs, or mite feces to examine under the microscope.
- In some cases, a skin biopsy is done.
Treatment
HOME CARE
- Before treatment, wash clothes and underwear, towels, bedding and sleepwear in hot water and dry at 140°F (60°C) or higher. Dry cleaning also works. If washing or dry cleaning can't be done, keep these items away from the body for at least 72 hours. Away from the body, the mites will die.
- Vacuum carpets and upholstered furniture.
- Use calamine lotion or soak in a cool bath to ease itching.
- Take an oral antihistamine if your provider recommends it for very bad itching.
MEDICINES FROM YOUR HEALTH CARE PROVIDER
The whole family and sexual partners of infected people should be treated, even if they do not have symptoms.
Creams or lotions prescribed by your provider are needed to treat scabies.
- The medicine most often used is permethrin 5%.
- Other medicines include benzyl benzoate, sulfur in petrolatum, and crotamiton.
Apply the medicine all over your body. The treatment is typically repeated in 1 week.
For hard to treat cases, your provider may also prescribe a pill known as ivermectin.
Outlook (Prognosis)
Itching may continue for 2 weeks or more after treatment ends. It will most likely disappear if you follow your provider's treatment plan.
Most cases of scabies can be cured without any long-term problems. A severe case with a lot of scaling or crusting may be a sign that the person has a weakened immune system.
Possible Complications
Intense scratching can cause a secondary skin infection, such as impetigo.
When to Contact a Medical Professional
Contact your provider if:
- You have symptoms of scabies.
- A person you have been in close contact with has been diagnosed with scabies.
Alternative Names
Human scabies; Sarcoptes scabiei
References
Diaz JH. Scabies. In: Blaser MJ, Cohen JI, Holland SM, et al. eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 10th ed. Philadelphia, PA: Elsevier; 2026:chap 299.
James WD. Parasitic infestations, stings, and bites. In: James WD, ed. Andrews' Diseases of the Skin: Clinical Dermatology. 14th ed. Philadelphia, PA: Elsevier; 2026:chap 15.
Review Date 11/20/2025
Updated by: Ramin Fathi, MD, FAAD, Director, Phoenix Surgical Dermatology Group, Phoenix, AZ. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.