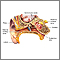
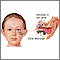
Swimmer's ear is inflammation, irritation, or infection of the outer ear and ear canal. The medical term for swimmer's ear is otitis externa.
Swimmer's ear may be sudden and short-term (acute) or long-term (chronic).
Causes
Swimmer's ear is more common among children in their teens and young adults. It may occur with a middle ear infection or a respiratory infection such as a cold.
Swimming in unclean water can lead to swimmer's ear. Bacteria commonly often found in water can cause ear infections. Rarely, the infection may be caused by a fungus.
Other causes of swimmer's ear include:
- Scratching the ear or inside the ear which can damage the skin of the ear canal
- Getting something stuck in the ear
Trying to clean (wax from the ear canal) with cotton swabs or small objects can also damage the skin.
Long-term (chronic) swimmer's ear may be due to:
Symptoms
Symptoms of swimmer's ear include:
- Drainage from the ear -- yellow, yellow-green, pus-like, or foul smelling
- Ear pain, which may get worse when you pull on the outer ear
- Hearing loss
- Itching of the ear or ear canal
Exams and Tests
The health care provider will look inside your ears. The ear canal area will look red and swollen. The skin inside the ear canal may be scaly or shedding.
Touching or moving the outer ear will increase the pain. The eardrum may be hard to see because of a swelling in the outer ear. The eardrum may have a hole in it. This is called a perforation.
A sample of fluid may be removed from the ear and sent to a lab to look for bacteria or fungus.
Treatment
In most cases, you will need to use antibiotic ear drops for 10 to 14 days. If the ear canal is very swollen, a wick may be put into the ear. The wick will allow the drops to travel to the end of the canal. Your provider can show you how to do this.
Other treatments may include:
- Antibiotics taken by mouth if you have a middle ear infection or infection that spreads beyond the ear
- Corticosteroids to reduce itching and inflammation
- Pain medicine, such as acetaminophen (Tylenol) or ibuprofen (Advil, Motrin)
- Vinegar (acetic acid) ear drops
People with chronic swimmer's ear may need long-term or repeated treatment. This will avoid complications.
Placing something warm against the ear may reduce pain.
Outlook (Prognosis)
Swimmer's ear most often gets better with the proper treatment.
Possible Complications
The infection may spread to other areas around the ear, including the skull bone. In older people or those who have diabetes or a condition that weakens the immune system, the infection may become severe. This condition is called malignant otitis externa. This condition is treated with high-dose antibiotics given through a vein.
When to Contact a Medical Professional
Contact your provider if:
- You develop any symptoms of swimmer's ear
- You notice any drainage coming from your ears
- Your symptoms get worse or continue despite treatment
- You have new symptoms, such as fever or pain and redness of the skull behind the ear
Prevention
These steps can help protect your ears from further damage:
- DO NOT scratch the ears or insert cotton swabs or other objects in the ears.
- Keep ears clean and dry, and DO NOT let water enter the ears when showering, shampooing, or bathing.
- Dry your ear very well after it has gotten wet.
- Avoid swimming in polluted water.
- Use earplugs when swimming.
- Try mixing 1 drop of alcohol with 1 drop of white vinegar and placing the mixture into the ears after they get wet. The alcohol and acid in the vinegar help prevent bacterial growth.
Alternative Names
Ear infection - outer ear - acute; Otitis externa - acute; Chronic swimmer's ear; Otitis externa - chronic; Ear infection - outer ear - chronic
References
American Speech-Language Hearing Association website. Swimmer's ear (otitis externa). www.asha.org/public/hearing/Swimmers-Ear/. Accessed August 1, 2024.
Haddad J. External otitis (otitis externa). In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 679.
Naples JG, Brant JA, Ruckenstein MJ. Infections of the external ear. In: Flint PW, Francis HW, Haughey BH, et al, eds. Cummings Otolaryngology: Head and Neck Surgery. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 138.
Review Date 7/16/2024
Updated by: Neil K. Kaneshiro, MD, MHA, Clinical Professor of Pediatrics, University of Washington School of Medicine, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.