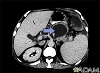
A pancreatic pseudocyst is a fluid-filled sac in the abdomen that arises from the pancreas. It may also contain tissue from the pancreas, enzymes, and blood.
Causes
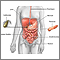
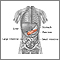
The pancreas is an organ located behind the stomach. It produces chemicals (called enzymes) needed to digest food. It also produces the hormones insulin and glucagon.
Pancreatic pseudocysts most often develop after an episode of severe acute pancreatitis. Pancreatitis happens when your pancreas gets inflamed. There are many causes of this problem.
This problem may sometimes occur:
- In someone with long-term (chronic) swelling of the pancreas (pancreatitis), most often due to alcohol abuse
- After trauma to the belly, more often in children
The pseudocyst happens when the ducts (tubes) in the pancreas are damaged and fluid with enzymes cannot drain.
Symptoms
Symptoms can occur within days to months after an attack of pancreatitis. They include:
- Bloating of the abdomen
- Constant pain or deep ache in the abdomen, which may also be felt in the back
- Nausea and vomiting
- Loss of appetite
- Difficulty eating and digesting food
Exams and Tests
The health care provider will feel your abdomen for a pseudocyst. It will feel like a lump in the middle or left upper abdomen.
Tests that may help detect a pancreatic pseudocyst include:
Treatment
The treatment depends on the size of the pseudocyst and whether it is causing symptoms. Many pseudocysts go away on their own. Those that remain for more than 6 weeks and are larger than 5 centimeters (about 2 inches) in diameter may need treatment. However, size and duration do not always mean treatment is needed, especially in a person without any symptoms and whose pseudocyst is not getting bigger.
Possible treatments include:
- Drainage through the skin using a needle, most often guided by a CT scan.
- Endoscopic-assisted drainage using an endoscope (endoscopic ultrasound). In this, a tube containing a camera and a light is passed down into the stomach.
- Surgical drainage of the pseudocyst. A connection is made between the cyst and the stomach or small intestine. This may be done using a laparoscope (a thin, tube-like instrument with a camera and light on one end).
Outlook (Prognosis)
The outcome is generally good with treatment. It is important to make sure that it is not pancreatic cancer that starts in a cyst, which has a worse outcome.
Possible Complications
Complications may include:
- A pancreatic abscess can develop if the pseudocyst becomes infected.
- The pseudocyst can break open (rupture). This can be a serious complication because shock and excess bleeding (hemorrhage) may develop.
- The pseudocyst may press down on (compress) nearby organs.
When to Contact a Medical Professional
If you are known to have a pseudocyst, rupture of the pseudocyst is a medical emergency. Go to the emergency room or call 911 or the local emergency number if you develop symptoms of bleeding or shock, such as:
- Fainting
- Fever and chills
- Rapid heartbeat
- Severe abdominal pain
Prevention
The way to prevent pancreatic pseudocysts is by preventing pancreatitis. If pancreatitis is caused by gallstones, you may have surgery to remove the gallbladder (cholecystectomy).
When pancreatitis occurs due to alcohol use, you must stop drinking alcohol to prevent future attacks.
When pancreatitis occurs due to high blood triglycerides, this condition should be treated.
Alternative Names
Pancreatitis - pseudocyst
References
Forsmark CE. Pancreatitis. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 130.
Javed AA, Lafaro KJ. Pancreas: Management of pancreatic pseudocyst. In: Cameron JL, Cameron AM, eds. Current Surgical Therapy. 14th ed. Philadelphia, PA: Elsevier; 2023:568-573.
Van Buren G, Fisher WE. Acute and chronic pancreatitis. In: Kellerman RD, Heidelbaugh JJ, Lee EM, eds. Conn's Current Therapy 2025. Philadelphia, PA: Elsevier; 2025:179-186.
Vege SS. Acute pancreatitis. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease: Pathophysiology/Diagnosis/Management. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 58.
Review Date 10/20/2025
Updated by: Todd Eisner, MD, Private practice specializing in Gastroenterology in Boca Raton and Delray Beach, Florida at Gastroenterology Consultants of Boca Raton. Affiliate Assistant Professor, Florida Atlantic University School of Medicine. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.