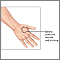
An animal bite can break, puncture, or tear the skin. Bites that break the skin put you at risk for infections.
Causes
Most animal bites come from pets. Dog bites are common and most often happen to children. Compared with adults, children are much more likely to be bitten on the face, head, or neck.
Cat bites are less common but have a higher risk for infection. Cat teeth are longer and sharper, which can cause deeper puncture wounds. Most other animal bites are caused by stray or wild animals, such as skunks, raccoons, foxes, and bats.
Bites that cause a puncture wound are more likely to become infected. Some animals are infected with a virus that can cause rabies. Rabies is rare but is often deadly.
Symptoms
Pain, bleeding, numbness and tingling may occur with any animal bite.
The bite may also result in:
- Breaks or major cuts in the skin, with or without bleeding
- Bruising (discoloration of the skin)
- Crushing injuries that can cause severe tissue tears and scarring
- Puncture wounds
- Tendon or joint injury resulting in decreased motion and function of the injured tissue
Wound Care
You should get medical attention within 24 hours for any bite that breaks the skin:
- You may need stitches for deeper wounds.
- You may need to get a tetanus shot.
- You may need to take antibiotics due to the risk for infection or receive antibiotics through a vein (IV) if the infection has spread.
- You may need surgery to repair the damage from a bad bite.
If you are caring for someone who was bitten:
- Calm and reassure the person.
- Wash your hands thoroughly with soap and water before treating the wound.
- If the wound is bleeding, put on latex gloves if you have them.
- Wash your hands again afterward.
To care for a bite wound:
- Stop the wound from bleeding by applying direct pressure with a clean, dry cloth.
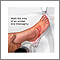
- Wash the wound. Use mild soap and warm, running water. Rinse the bite for 3 to 5 minutes.
- Apply an antibacterial ointment to the wound. This may help reduce the risk for infection.
- Put on a dry, sterile bandage.
- Contact your health care provider right away if the bite is on your neck, head, face, hand, fingers, or feet.
When to Call Animal Control
You should contact animal control or your local police if you are bitten by:
- An animal that behaves in an odd way
- An unknown pet or a pet that has not had a rabies vaccination
- A stray or wild animal
Tell them what the animal looks like and where it is. They will decide whether the animal needs to be captured and isolated.
Possible Complications
Most animal bites will heal without developing infection or decreased tissue function. Ask your provider if you should take an antibiotic to reduce the chance of an infection.
Some wounds will require surgery to properly clean and close, and even some minor bites may need stitches. Deep or extensive wounds may result in significant scarring.
Complications from bite wounds include:
- An infection that spreads quickly
- Damage to tendons or joints
An animal bite is more likely to become infected in people who have:
- Weakened immune systems due to medicines or disease
- Diabetes
- Peripheral arterial disease (arteriosclerosis, or poor circulation)
Getting a rabies shot right after you are bitten can protect you from the disease.
How to Prevent Animal Bites
To prevent animal bites:
- Teach children not to approach strange animals.
- Do not provoke or tease animals.
- Do not go near an animal that is acting strangely or aggressively. It may have rabies. Do not try to catch the animal yourself.
When to Call the Doctor
Wild animals and unknown pets could be carrying rabies. If you have been bitten by a wild or stray animal, contact your provider right away. See your provider within 24 hours for any bite that breaks the skin.
Contact your provider or go to the emergency room if:
- There is swelling, redness, or pus draining from the wound.
- The bite is on the head, face, neck, hands, or feet.
- The bite is deep or large.
- You see exposed muscle or bone.
- You are not sure if the wound needs stitches.
- The bleeding does not stop after a few minutes. For serious bleeding, call 911 or the local emergency number.
- You have not had a tetanus shot in 5 years.
- You notice red streaks that spread out from the wound.
Alternative Names
Bites - animals - self-care
References
Eilbert WP. Mammalian bites. In: Walls RM, ed. Rosen's Emergency Medicine: Concepts and Clinical Practice. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 52.
Goldstein EJC, Abrahamian FM. Bites. In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 315.
Review Date 4/3/2024
Updated by: Jesse Borke, MD, CPE, FAAEM, FACEP, Attending Physician at Kaiser Permanente, Orange County, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.