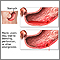
A peptic ulcer is an open sore or raw area in the lining of the stomach (gastric ulcer) or upper part of the small intestine (duodenal ulcer). This article describes how to care for yourself after you have been treated by your health care provider for this condition.
What to Expect at Home
You have peptic ulcer disease (PUD). You may have had tests to help diagnose your ulcer. One of these tests may have been to look for bacteria in your stomach called Helicobacter pylori (H pylori). This type of infection is a common cause of peptic ulcers.
Most peptic ulcers will heal within 4 to 6 weeks after treatment begins. Do not stop taking the medicines you have been prescribed, even if symptoms go away quickly.
Diet and Lifestyle
People with PUD should eat a healthy balanced diet.
It does not help to eat more often or increase the amount of milk and dairy products you consume. These dietary changes may even cause more stomach acid.
- Avoid foods and drinks that cause discomfort for you. For many people these include alcohol, coffee, caffeinated soda, fatty foods, chocolate, and spicy foods.
- Avoid eating late night snacks.
Other things you can do to ease your symptoms and help healing include:
- If you smoke or chew tobacco, try to quit. Tobacco will slow the healing of your ulcer and increase the chance that the ulcer will come back. Talk to your doctor about getting help for quitting tobacco use.
- Try to reduce your stress level and learn ways to better manage stress.
Avoid drugs such as aspirin, ibuprofen (Advil, Motrin IB), or naproxen (Aleve, Naprosyn). Take acetaminophen (Tylenol) to relieve pain. Take all medicines with plenty of water.
Medicines
The standard treatment for a peptic ulcer and an H pylori infection uses a combination of medicines that you take for 5 to 14 days.
- Most people will take two types of antibiotics and a proton pump inhibitor (PPI).
- These medicines may cause nausea, diarrhea, and other side effects. Do not just stop taking them without talking to your provider first.
If you have an ulcer without an H pylori infection, or one that is caused by taking aspirin or nonsteroidal anti-inflammatory drugs (NSAIDs), you will likely need to take a proton pump inhibitor for 8 weeks.
Taking antacids as needed between meals, and then at bedtime, may help healing also. Ask your provider about taking these medicines.
Talk to your provider about your medicine choices if your ulcer was caused by aspirin, ibuprofen, or other NSAIDs. You may be able to take a different anti-inflammatory medicine. Or, your provider may have you take a medicine called misoprostol or a PPI to prevent future ulcers while taking an NSAID.
Follow-up
You will have follow-up visits to see how your ulcer is healing especially if the ulcer was in the stomach.
Your provider may want to perform an upper endoscopy after treatment if the ulcer was in your stomach. This is to make sure healing has taken place and there are no signs of cancer.
You will also need follow-up testing to check that the H pylori bacteria are gone. You should wait at least 2 weeks after therapy is completed to be retested. Test results before that time may not be accurate.
When to Call the Doctor
Get medical help right away if you:
- Develop sudden, sharp abdominal pain
- Have a rigid, hard abdomen that is tender to the touch
- Have symptoms of shock, such as fainting, excessive sweating, or confusion
- Vomit blood
- See blood in your stool (maroon, dark, or tarry black stools)
Contact your provider if:
- You feel dizzy or light-headed
- You have ulcer symptoms
- You feel full after eating a small meal portion
- You experience unintentional weight loss
- You are vomiting
- You lose your appetite
Alternative Names
Ulcer - peptic - discharge; Ulcer - duodenal - discharge; Ulcer - gastric - discharge; Duodenal ulcer - discharge; Gastric ulcer - discharge; Dyspepsia - ulcer - discharge; Peptic ulcer discharge
Images
References
Chan FKL, Lau JYW. Peptic ulcer disease. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 53.
Cover TL, Blaser MJ. Helicobacter pylori and other gastric Helicobacter species. In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 217.
Kuipers EJ. Acid peptic disease. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 125.
Vincent K. Gastritis and peptic ulcer disease. In: Kellerman RD, Heidelbaugh JJ, Lee EM, eds. Conn's Current Therapy 2025. Philadelphia, PA: Elsevier; 2025:232-235.
Review Date 4/21/2025
Updated by: Todd Eisner, MD, Private practice specializing in Gastroenterology in Boca Raton and Delray Beach, Florida at Gastroenterology Consultants of Boca Raton. Affiliate Assistant Professor, Florida Atlantic University School of Medicine. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.