Acute flaccid myelitis (AFM) is a rare condition that affects the nervous system. Inflammation of the gray matter in the spinal cord leads to muscle weakness and paralysis.
AFM is usually caused by an infection with a virus. While AFM is rare, there has been a slight increase in cases of AFM since 2014. Most new cases have occurred in children or young adults.
Causes
AFM usually occurs after a cold, fever, or gastrointestinal illness.
Different kinds of viruses may be the cause of AFM. These include:
- Enteroviruses (poliovirus and non-poliovirus)
- West Nile virus and similar viruses such as Japanese encephalitis virus and Saint Louis encephalitis virus
- Adenoviruses
It is unclear why certain viruses trigger AFM, or why some people develop the condition and others don't.
Environmental toxins also can cause AFM. In many cases, a cause is never found.
Symptoms
A fever or a respiratory illness is often present before weakness and other symptoms begin.
AFM symptoms often start with sudden muscle weakness and loss of reflexes in an arm or leg. Symptoms may progress rapidly over a few hours to days. Other symptoms may include:
- Facial droop or weakness
- Drooping eyelids
- Difficulty moving the eyes
- Slurred speech or difficulty swallowing
Some people may have:
- Stiffness in the neck
- Pain in the arms or legs
- Inability to pass urine
Severe symptoms include:
- Respiratory failure, when muscles involved in breathing become weak
- Serious nervous system problems, which may lead to death
Exams and Tests
Your health care provider will take your medical history and vaccination history to know if you are up-to-date with your polio vaccines. Unvaccinated individuals who are exposed to poliovirus are at higher risk for AFM. Your provider also may want to know if within the last 4 weeks you have:
- Traveled
- Had a cold or the flu or a stomach bug
- Had a fever 100°F (37.8°C) or higher
Your provider will do a physical exam. Tests that may be done include:
- MRI of spine and MRI of the brain to view lesions in the gray matter
- Nerve conduction velocity test
- Electromyography (EMG)
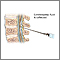
- Cerebrospinal fluid (CSF) analysis to check if white blood cells are elevated
Your provider also may take stool, blood, and saliva samples to test.
Treatment
There is no specific treatment for AFM. You may be referred to a doctor specializing in disorders of the nerves and nervous system (neurologist). The neurologist will likely help treat your symptoms.
A number of medicines and treatments that work on the immune system have been tried but have not been found to help.
You may need physical therapy to help restore muscle function.
Outlook (Prognosis)
The long-term outlook of AFM is not known.
Possible Complications
Complications of AFM include:
- Muscle weakness and paralysis
- Loss of limb function
When to Contact a Medical Professional
Contact your provider right away if you or your child have:
- Sudden weakness in the arms or legs or difficulty moving the head or face
- Any other symptom of AFM
Prevention
There is no known way to prevent AFM. Having a polio vaccine may help reduce the risk of AFM related to the poliovirus.
Take these steps to help avoid viral infections:
- Wash hands frequently with soap and water, especially before eating.
- Avoid close contact with people who have a viral infection.
- Use mosquito repellants when going outdoors to prevent mosquito bites.
To learn more and get recent updates, go to the CDC webpage about AFM at www.cdc.gov/acute-flaccid-myelitis/index.html.
Alternative Names
Acute flaccid myelitis; AFM; Polio-like syndrome; Acute flaccid paralysis; Acute flaccid paralysis with anterior myelitis; Anterior myelitis; Enterovirus D68; Enterovirus A71
References
Centers for Disease Control and Prevention website. Acute flaccid myelitis (AFM). www.cdc.gov/acute-flaccid-myelitis/index.html. Updated May 9, 2024. Accessed November 8, 2024.
Kapadia RK, Pastula DM, Glaser CA. Parainfectious and postinfectious neurologic syndromes. In: Long SS, Prober CG, Fischer M, Kimberlin DW, eds. Principles and Practice of Pediatric Infectious Diseases. 6th ed. Philadelphia, PA: Elsevier; 2023:chap 45.
Messacar K, Abzug MJ. Enteroviruses and parechoviruses. In: Long SS, Prober CG, Fischer M, Kimberlin DW, eds. Principles and Practice of Pediatric Infectious Diseases. 6th ed. Philadelphia, PA: Elsevier; 2023:chap 236.
Review Date 10/23/2024
Updated by: Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School at Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.