Nasopharyngeal culture is a test that examines a sample of secretions from the uppermost part of the throat, behind the nose, to detect organisms that can cause disease.
How the Test is Performed
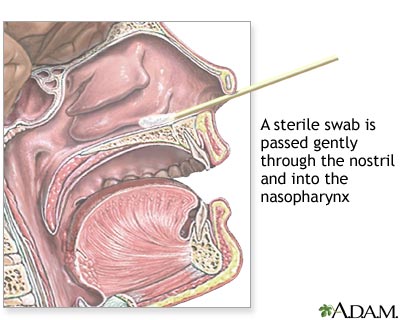
You will be asked to cough before the test begins and then tilt your head back. A sterile cotton-tipped swab is gently passed through a nostril and into your nasopharynx. This is the part of the pharynx that covers the roof of the mouth. The swab is quickly rotated and removed. The sample is sent to a lab. There, it is placed in a special dish (culture). It is then watched to see if bacteria, viruses, or other disease-causing organisms grow.
How to Prepare for the Test
No special preparation is needed.
How the Test will Feel
You may have slight discomfort and may gag.
Why the Test is Performed
The test identifies viruses and bacteria that cause upper respiratory tract symptoms. These include:
- Bordetella pertussis, the bacteria that cause whooping cough.
- Neisseria meningitidis, the bacteria that cause meningococcal meningitis.
- Staphylococcus aureus, the bacteria that cause staph infections.
- Methicillin-resistant Staphylococcus aureus (MRSA).
- Viral infections such as influenza, respiratory syncytial virus, or SARS-CoV-2 (COVID-19). This is the most common reason the test is used.
The culture may be used to help determine which antibiotic is appropriate to treat an infection due to bacteria.
Normal Results
The presence of organisms commonly found in the nasopharynx is normal.
What Abnormal Results Mean
The presence of any disease-causing virus, bacteria, or fungus means these organisms may be causing your infection.
Sometimes, organisms like Staphylococcus aureus can be present without causing disease. This test can help identify resistant strains of this organism (MRSA) so that people can be isolated when necessary.
Risks
A minor nose bleed can occur, but it is rare.
Alternative Names
Culture - nasopharyngeal; Swab for respiratory viruses; Swab for staph carriage
Images
References
Nayak JL, Treanor JJ. Influenza viruses, including avian influenza and swine influenza. In: Blaser MJ, Cohen JI, Holland SM, et al, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 10th ed. Philadelphia, PA: Elsevier; 2026:chap 172.
Patel R. The clinician and the microbiology laboratory: test ordering, specimen collection, and result interpretation. In: Blaser MJ, Cohen JI, Holland SM, et al, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 10th ed. Philadelphia, PA: Elsevier; 2026:chap 16.
Roginski MA, Atchinson PR. Upper respiratory tract infections. In: Walls RM, ed. Rosen's Emergency Medicine: Concepts and Clinical Practice. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 61.
Review Date 11/6/2025
Updated by: Jacob Berman, MD, MPH, Associate Professor of Medicine, Division of General Internal Medicine, University of Washington School of Medicine, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.