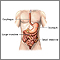
Gastrointestinal (GI) bleeding refers to any bleeding that starts in the GI tract.
Bleeding may come from any site along the GI tract, but is often divided into:
- Upper GI bleeding: The upper GI tract includes the esophagus (the tube from the mouth to the stomach), stomach, and first part of the small intestine (duodenum).
- Lower GI bleeding: The lower GI tract includes most of the small intestine, and the entire large intestine, rectum, and anus.
Considerations
The amount of GI bleeding may be so small that it can only be detected on a lab test, such as the fecal occult blood test or fecal immunochemical test. Other signs of GI bleeding include:
- Dark, tarry stools
- Larger amounts of blood passed from the rectum
- Small amounts of blood in the toilet bowl, on toilet paper, or in streaks on stool (feces)
- Vomiting blood
Massive bleeding from the GI tract can be dangerous or even life threatening. However, even very small amounts of bleeding that occur over a long period of time can lead to problems such as anemia or low blood counts.
Once a bleeding site is found, many therapies are available to stop the bleeding or treat the cause.
Causes
GI bleeding may be due to conditions that are not serious, including:
GI bleeding may also be a sign of more serious diseases and conditions. These may include cancers of the GI tract, such as:
- Cancer of the colon
- Cancer of the small intestine
- Cancer of the stomach
- Intestinal polyps (a pre-cancerous condition)
Other causes of GI bleeding may include:
- Abnormal blood vessels in the lining of the intestines (also called angiodysplasia)
- Bleeding diverticulum, or diverticulosis
- Crohn disease or ulcerative colitis
- Esophageal or gastric varices
- Esophagitis
- Gastric (stomach) ulcer
- Intussusception (bowel telescoped on itself)
- Mallory-Weiss tear
- Meckel diverticulum
- Radiation injury to the bowel
Home Care
There are home stool tests for microscopic blood that may be recommended for people with anemia or for colon cancer screening.
When to Contact a Medical Professional
Contact your health care provider if you notice small amounts of blood in your stool to discuss the next step.
Call 911 or go to the nearest emergency room if:
- You have black, tarry stools (this may be a sign of GI bleeding)
- You have a lot of blood in your stool
- You vomit blood or you vomit material that looks like coffee grounds
- You are lightheaded or dizzy from the bleeding
- You have chest pain or trouble breathing
- You have severe abdominal pain along with bleeding
What to Expect at Your Office Visit
Your provider may discover GI bleeding during an exam at your office visit.
GI bleeding can be an emergency condition that requires immediate medical care. Treatment may involve:
- Blood transfusions.
- Fluids and medicines through a vein.
- Esophagogastroduodenoscopy (EGD). A thin tube with a camera on the end is passed through your mouth into your esophagus, stomach, and small intestine.
- A tube that is placed through your mouth into the stomach to drain the stomach contents (gastric lavage).
- Colonoscopy. A thin tube with a camera on the end passed through the rectum to look at the lower GI tract.
Once your condition is stable, you will have a physical exam and a detailed exam of your abdomen. You will also be asked questions about your symptoms, including:
- When did you first notice symptoms?
- Did you have black, tarry stools or red blood in the stools?
- Have you vomited blood?
- Did you vomit material that looks like coffee grounds?
- Do you have a history of peptic or duodenal ulcers?
- Have you ever had symptoms like this before?
- What other symptoms do you have?
Tests that may be done include:
- Abdominal CT scan or CT angiography
- Abdominal MRI scan or MR angiography
- Abdominal x-ray
- Angiography
- Bleeding scan (tagged red blood cell scan)
- Blood clotting tests
- Capsule endoscopy (camera shaped like a pill that is swallowed to look at the small intestine)
- Colonoscopy
- Complete blood count (CBC), clotting tests, platelet count, and other laboratory tests
- EGD
- Enteroscopy
- Sigmoidoscopy
Alternative Names
Lower GI bleeding; GI bleeding; Upper GI bleeding; Hematochezia
References
DeGeorge LM, Nable JV. Gastrointestinal bleeding. In: Walls RM, ed. Rosen's Emergency Medicine: Concepts and Clinical Practice. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 26.
Kovacs TO, Jensen DM. Gastrointestinal hemorrhage. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 121.
Savides TJ, Jensen DM. Gastrointestinal bleeding. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 20.
Review Date 1/24/2025
Updated by: Jenifer K. Lehrer, MD, Gastroenterologist, Philadelphia, PA. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.