Tonsillectomy is a surgery to remove the tonsils.
The tonsils are glands at the back of your throat. The tonsils are often removed along with the adenoid glands. The latter surgery is called adenoidectomy and is most often done in children.
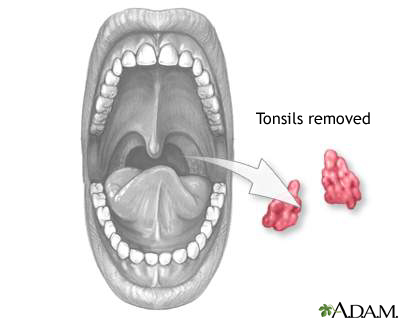
Description
The surgery is done while your child is under general anesthesia. Your child will be asleep and pain-free.
- The surgeon will place a small tool into your child's mouth to hold it open.
- The surgeon then cuts, burns, or shaves away the tonsils. The wounds heal naturally without stitches.
After surgery, your child will stay in the recovery room until he or she is awake and can breathe easily, cough, and swallow. Most children go home several hours after this surgery.
Why the Procedure is Performed
The tonsils help protect against infections. But children with large tonsils may have problems breathing at night. The tonsils may also trap excess bacteria which can lead to frequent or very painful sore throats. In either of these cases, your child's tonsils have become more harmful than protective.
You and your child's health care provider may consider a tonsillectomy if:
- Your child has infections often (7 or more times in 1 year, or 5 or more times each year over the last 2 years).
- Your child misses a lot of school.
- Your child has trouble breathing and does not sleep well because the tonsils block the airway (sleep apnea).
- Your child has an abscess or a growth on the tonsils.
- Your child gets frequent and bothersome tonsil stones.
Risks
The risks for any anesthesia are:
- Reaction to medicines
- Breathing problems
The risks for any surgery are:
- Bleeding
- Infection
Rarely, bleeding after surgery can go unnoticed and becomes apparent when the child vomits blood. Some children will also be unable to drink enough liquids to maintain adequate hydration and may require an IV (intravenous) fluids.
Another risk includes injury to the uvula (soft palate).
Before the Procedure
Your child's surgeon may ask your child to have:
- Blood tests (complete blood count, electrolytes, and clotting factors)
- A physical exam and medical history
Always tell your child's surgeon what medicines your child is taking. Include any medicines, herbs, or vitamins you bought without a prescription.
During the days before the surgery:
- Ten days before the surgery, your child may be asked to stop taking aspirin, ibuprofen (Advil, Motrin), naproxen (Aleve, Naprosyn), warfarin (Coumadin), and other medicines like these.
- Ask your child's surgeon which medicines your child should still take on the day of the surgery.
On the day of the surgery:
- Your child will most often be asked not to drink or eat anything for several hours before the surgery.
- Give your child any medicines you have been told to give with a small sip of water.
- You will be told when to arrive at the hospital.
After the Procedure
A tonsillectomy is most often done in a hospital or surgery center. Your child will go home the same day as the surgery. Children rarely need to stay overnight in the hospital for observation.
Complete recovery takes about 1 to 2 weeks. During the first week, your child should avoid people who are sick. It will be easier for your child to become infected during this time. Your child should also avoid playing sports or any strenuous activity for 2 weeks after surgery to avoid increasing the risk of bleeding.
Outlook (Prognosis)
After surgery, the number of throat infections is most often lower, but your child may still get some.
Alternative Names
Tonsils removal; Tonsillitis - tonsillectomy; Pharyngitis - tonsillectomy; Sore throat - tonsillectomy
Patient Instructions
References
Goldstein NA. Evaluation and management of pediatric obstructive sleep apnea. In: Flint PW, Francis HW, Haughey BH, et al, eds. Cummings Otolaryngology: Head and Neck Surgery. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 186.
Mitchell RB, Archer SM, Ishman SL, et al. Clinical Practice Guideline: tonsillectomy in children (update). Otolaryngol Head Neck Surg. 2019;160(2):187-205. PMID: 30921525 pubmed.ncbi.nlm.nih.gov/30921525/.
Zur KB. Tonsils and adenoids. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 431.
Review Date 7/28/2025
Updated by: Ashutosh Kacker, MD, FACS, Professor of Clinical Otolaryngology, Weill Cornell Medical College, and Attending Otolaryngologist, New York-Presbyterian Hospital, New York, NY. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.