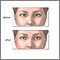
Eye muscle repair is surgery to correct eye muscle problems that cause strabismus (crossed eyes).
Description
The goal of this surgery is to restore the eye muscles to a proper position. This will help the eyes move correctly.
Eye muscle surgery is most often done on children. However, adults who have similar eye problems may also have it done. Children will most often have general anesthesia for the procedure. They will be asleep and will not feel pain.
Depending on the problem, one or both eyes may need surgery.
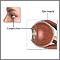
After the anesthesia has taken effect, the eye surgeon makes a small surgical cut in the clear tissue covering the white of the eye. This tissue is called the conjunctiva. Then the surgeon will locate one or more of the eye muscles that needs surgery. Sometimes the surgery strengthens the muscle, and sometimes it weakens it.
- To strengthen a muscle, a section of the muscle or tendon may be removed to make it shorter. This step in the surgery is called a resection.
- To weaken a muscle, it is reattached to a point farther toward the back of the eye. This step is called a recession.
The surgery for adults is similar. In most cases, adults are awake, but are given medicine to numb the area and help them relax.
When the procedure is done on adults, an adjustable stitch is used on the weakened muscle so that minor changes can be made later that day or the next day. This technique often has a very good outcome.
Why the Procedure is Performed
Strabismus is a disorder in which the two eyes do not line up in the same direction. Therefore, the eyes do not focus on the same object at the same time. The condition is more commonly known as "crossed eyes."
Surgery may be recommended when strabismus does not improve with glasses or eye exercises.
Risks
Risks for any anesthesia are:
- Reactions to anesthesia medicines
- Breathing problems
Risks for any surgery are:
- Bleeding
- Infection
Some risks for this surgery include:
- Wound infections
- Damage to the eye (rare)
- Permanent double vision (rare)
Before the Procedure
Your child's eye surgeon may ask for:
- A complete medical history and physical exam before the procedure
- Orthoptic measurements (eye movement measurements)
Always tell your child's health care provider:
- What medicines your child is taking
- What medicines, herbs, or vitamins you bought without a prescription that your child is taking
- About any allergies your child may have to any medicines, latex, tape, soaps or skin cleaners
During the days before the surgery:
- About 10 days before the surgery, you may be asked to stop giving your child aspirin, ibuprofen (Advil, Motrin), warfarin (Coumadin), and any other blood thinners.
- Ask your child's eye surgeon which medicines your child should still take on the day of the surgery.
On the day of the surgery:
- Your child will often be asked not to drink or eat anything for several hours before the surgery.
- Give your child any medicines your surgeon told you to give your child with a small sip of water.
- Your child's surgeon or nurse will tell you when to arrive for the surgery.
- The surgeon will make sure your child is healthy enough for surgery and does not have any signs of illness. If your child is ill, the surgery may be delayed.
After the Procedure
Most of the time, the surgery does not need an overnight stay in the hospital. The eyes are most often straight right after surgery.
While recovering from the anesthesia and in the first few days after surgery, your child should avoid rubbing their eyes. Your surgeon will show you how to prevent your child from rubbing their eyes.
After a few hours of recovery, your child may go home. You should have a follow-up visit with the eye surgeon 1 to 2 weeks after the surgery.
To prevent infection, you will probably need to put drops or ointment in your child's eyes.
Outlook (Prognosis)
Eye muscle surgery does not fix the poor vision of a lazy (amblyopic) eye. Your child may have to wear glasses or a patch.
In general, the younger a child is when the operation is performed, the better the result. Your child's eyes should look normal a few weeks after the surgery.
Alternative Names
Repair of cross-eye; Resection and recession; Strabismus repair; Extraocular muscle surgery
Patient Instructions
References
Coats DK, Olitsky SE. Strabismus surgery. In: Lyons CJ, Lambert SR, eds. Taylor and Hoyt's Pediatric Ophthalmology and Strabismus. 6th ed. Philadelphia, PA: Elsevier; 2023:chap 88.
Feuillade V, Bourcier T, Gaucher D, Speeg C, Sauer A. The effect of strabismus surgery on the learning abilities of school-aged children. Acta Ophthalmol. 2023:101(5):546-552. PMID: 36691981 pubmed.ncbi.nlm.nih.gov/36691981/.
Heidary G, Aakalu VK, Binenbaum G, et al. Adjustable sutures in the treatment of strabismus: a report by the American Academy of Ophthalmology. Ophthalmology. 2022;129(1):100-109. PMID: 34446304 pubmed.ncbi.nlm.nih.gov/34446304/.
Olitsky SE, Marsh JD. Disorders of eye movement and alignment. In: Kliegman RM, St. Geme JW, Blum NJ, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 663.
Robbins SL. Techniques of strabismus surgery. In: Yanoff M, Duker JS, eds. Ophthalmology. 6th ed. Philadelphia, PA: Elsevier; 2023:chap 11.13.
Review Date 8/5/2024
Updated by: Franklin W. Lusby, MD, Ophthalmologist, Lusby Vision Institute, La Jolla, CA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.