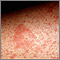
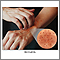
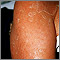
Erythroderma is widespread redness of the skin. It is accompanied by scaling, peeling, and flaking of the skin, and may include itching and hair loss.
Symptoms
Symptoms may include any of the following:
- Redness over 80% to 90% of the body
- Scaly skin patches
- Thickened skin
- Skin is itchy or painful with an odor
- Swelling of the arms or legs
- Fast heart beat
- Loss of fluids, leading to dehydration
- Loss of temperature regulation by the body
There may be secondary infections of the skin.
Exams and Tests
Your health care provider will ask about your symptoms and take your medical history. Your provider may do a skin exam with a dermatoscope. Most of the time, the cause can be identified after the exam.
If needed, the following tests may be ordered:
- Biopsy of the skin
- Allergy testing
- Other tests to find the cause of erythroderma
Treatment
Since erythroderma can quickly lead to serious complications, your provider will start treatment right away. This usually involves strong doses of steroid medicines to reduce inflammation.
Other treatments may include:
- Medicines to treat the underlying cause of erythroderma
- Antibiotics for any infection
- Dressings applied to the skin
- Ultraviolet light
- Correction of fluid and electrolyte balance
Outlook (Prognosis)
In serious cases, the person needs to be treated in the hospital.
Possible Complications
Complications may include:
- Secondary infections that can lead to sepsis (bodywide inflammatory response due to infection)
- Fluid loss that can result in dehydration and an imbalance of minerals (electrolytes) in the body
- Heart failure
When to Contact a Medical Professional
Contact your provider right away if:
- Symptoms get worse or do not get better, even with treatment.
- You develop new lesions.
Prevention
The risk for erythroderma may be reduced by following your provider's instructions on skin care.
Alternative Names
Exfoliative dermatitis; Dermatitis exfoliativa; Pruritus - exfoliative dermatitis; Pityriasis rubra; Red man syndrome; Exfoliative erythroderma
References
Calonje E, Brenn T, Lazar AJ, Billings SD. Spongiotic, psoriasiform and pustular dermatoses. In: Calonje E, Brenn T, Lazar AJ, Billings SD, eds. McKee's Pathology of the Skin. 5th ed. Philadelphia, PA: Elsevier; 2020:chap 6.
James WD. Papulosquamous, pustular and keratotic disorders. In: James WD, ed. Andrews' Diseases of the Skin. 14th ed. Philadelphia, PA: Elsevier; 2026:chap 11.
Whittaker S. Erythroderma. In: Bolognia JL, Schaffer JV, Cerroni L, eds. Dermatology. 5th ed. Philadelphia, PA: Elsevier; 2025:chap 10.
Review Date 1/28/2026
Updated by: Ramin Fathi, MD, FAAD, Director, Phoenix Surgical Dermatology Group, Phoenix, AZ. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.