Pityriasis rubra pilaris (PRP) is a rare skin disorder that causes inflammation and scaling (exfoliation) of the skin.
Causes
There are several subtypes of PRP. The cause is unknown, although genetic factors and an abnormal immune response may be involved. One subtype is associated with HIV/AIDS.
Symptoms
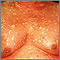
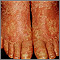
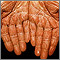
PRP is a chronic skin condition in which orange or salmon-colored scaly patches with thick skin develop on the hands and feet.
The scaly areas may cover much of the body. Small islands of normal skin (called islands of sparing) are seen within the areas of the scaly skin. The scaly areas may be itchy. There may be changes in the nails.
PRP can be severe. Although it's not life threatening, PRP can greatly reduce quality of life and limit activities of daily living.
Exams and Tests
Your health care provider will examine your skin. The diagnosis is usually made by the presence of the unique skin lesions (an abnormal area on the skin). Your provider may take samples (biopsies) of the affected skin to confirm the diagnosis and check for conditions that may look like PRP.
Treatment
Topical creams containing urea, lactic acid, retinoids, and steroids may help. More commonly, treatment includes pills taken by mouth such as isotretinoin, acitretin, or methotrexate. Exposure to ultraviolet light (light therapy) may also help. Medicines that affect the body's immune system are currently being studied and may be effective for PRP.
Support Groups
More information and support for people with PRP disorder and their families can be found at:
- National Institute of Health. Genetic and Rare Diseases Information Center -- rarediseases.info.nih.gov/diseases/7401/pityriasis-rubra-pilaris
- National Organization for Rare Disorders -- rarediseases.org/rare-diseases/pityriasis-rubra-pilaris/
When to Contact a Medical Professional
Contact your provider if you develop symptoms of PRP. Also contact your provider if you have the condition and symptoms worsen.
Alternative Names
PRP; Pityriasis pilaris; Lichen ruber acuminatus; Devergie disease
References
James WD. Papulosquamous, pustular and keratotic disorders. In: James WD, ed. Andrews' Diseases of the Skin: Clinical Dermatology. 14th ed. Philadelphia, PA: Elsevier; 2026:chap 10.
Patterson JW. Disorders of pigmentation. In: Patterson JW, ed. Weedon's Skin Pathology. 6th ed. Philadelphia, PA: Elsevier; 2025:chap 11.
Whittaker S. Erythroderma. In: Bolognia JL, Schaffer JV, Cerroni L, eds. Dermatology. 5th ed. Philadelphia, PA: Elsevier; 2025:chap 10.
Review Date 4/1/2025
Updated by: Elika Hoss, MD, Assistant Professor of Dermatology, Mayo Clinic, Scottsdale, AZ. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.