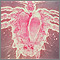
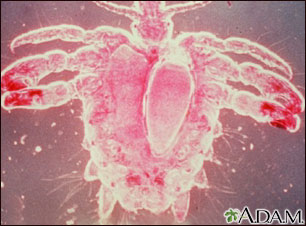
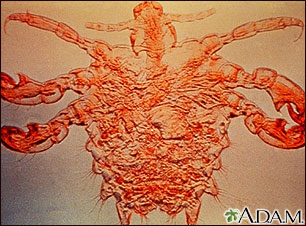
Pubic lice are tiny wingless insects that infect the pubic hair area and lay eggs there. These lice can also be found in armpit hair, eyebrows, mustache, beard, around the anus, and eyelashes (in children).
Causes
Pubic lice are most commonly spread during sexual activity.
Although not common, pubic lice can spread through contact with objects such as toilet seats, sheets, blankets, or bathing suits (that you may try on at a store).
Animals cannot spread public lice to humans.
Other types of lice include:
You are at greater risk for pubic lice if you:
- Have many sexual partners (high incidence in men who have sex with men)
- Have sexual contact with an infected person
- Share bedding or clothing with an infected person
Symptoms
Pubic lice cause itching in the area covered by pubic hair. Itching often gets worse at night. The itching may start soon after getting infected with lice, or it may not start for up to 2 to 4 weeks after contact.
Other symptoms can include:
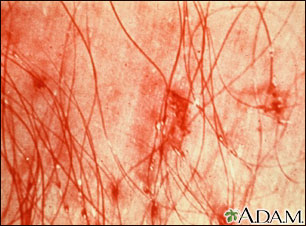
- Local skin reactions to the bites that cause the skin to turn red or bluish-gray
- Sores in the genital area due to bites and scratching
Exams and Tests
Your health care provider will do an exam to look for:
- The lice
- Small gray-white oval eggs (nits) attached to the hair shafts in the outer genital area
- Scratch marks or signs of a skin infection
Because pubic lice may cause an eye infection in young children, eyelashes should be looked at with a high-powered magnifying glass. Sexual transmission, and potential sexual molestation, should always be considered if pubic lice are found in children.
Adult lice are easy to identify with a special magnifying device called a dermatoscope. Pubic lice are often referred to as "the crabs" because of their appearance.
Teenagers and adults with pubic lice may need to be tested for other sexually transmitted infections (STIs).
Treatment
MEDICINES
Pubic lice are often treated with medicines that contain a substance called permethrin. To use this medicine:
- Thoroughly work the medicine into your pubic hair and surrounding area. Leave it on for at least 5 to 10 minutes, or as directed by your provider.
- Rinse well.
- Comb your pubic hair with a fine-toothed comb to remove eggs (nits). Applying vinegar to pubic hair before combing may help loosen the nits.
In case of eyelash infestation, applying soft paraffin three times daily for 1 to 2 weeks may help.
Most people need only one treatment. If a second treatment is needed, it should be done 4 days to 1 week later.
Over-the-counter medicines to treat lice include Rid, Nix, LiceMD, among others. Malathion lotion is another option.
Sexual partners should be treated at the same time.
OTHER CARE
While you are treating pubic lice:
- Wash and dry all clothing and bedding in hot water.
- Spray items that cannot be washed with a medicated spray that you can buy at the store. You can also seal items in plastic bags for 10 to 14 days to smother the lice.
Outlook (Prognosis)
The proper treatment, including thorough cleaning, should get rid of the lice.
Scratching can make the skin raw or cause a skin infection.
When to Contact a Medical Professional
Contact your provider for an appointment if:
- You or your sexual partner has symptoms of pubic lice
- You try over-the-counter lice treatments, and they are not effective
- Your symptoms continue after treatment
Prevention
Avoid sexual or intimate contact with people who have pubic lice until they have been treated.
Bathe or shower often and keep your bedding clean. Avoid trying on bathing suits while you are shopping. If you must try on swimwear, be sure to wear your underwear. This may prevent you from getting or spreading pubic lice.
Alternative Names
Pediculosis - pubic lice; Lice - pubic; Crabs; Pediculosis pubis; Phthirus pubis
References
Burkhart CN, Burkhart CG, Morrell DS. Infestations. In: Bolognia JL, Schaffer JV, Cerroni L, eds. Dermatology. 5th ed. Philadelphia, PA: Elsevier; 2025:chap 84.
Centers for Disease Control and Prevention website. Lice. Treatment of pubic lice. www.cdc.gov/lice/treatment/pubic-lice.html. Updated November 12, 2024. Accessed March 10, 2025.
Katsambas A, Dessinioti C. Parasitic diseases of the skin. In: Kellerman RD, Rakel DP, Heidelbaugh JJ, Lee EM, eds. Conn's Current Therapy 2024. Philadelphia, PA: Elsevier; 2024:1127-1132.
Kliegman RM, St. Geme JW, Blum NJ, et al. Arthropod bites and infestations. In: Kleigman RM, Blum NJ, Tasker RC, et al, eds. Nelson Textbook of Pediatrics. 22nd ed. Philadelphia, PA: Elsevier; 2025:chap 709.
Review Date 10/13/2024
Updated by: Ramin Fathi, MD, FAAD, Director, Phoenix Surgical Dermatology Group, Phoenix, AZ. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.