A tension headache is the most common type of headache. It is pain or discomfort in the head, scalp, or neck, and is often associated with muscle tightness in these areas.
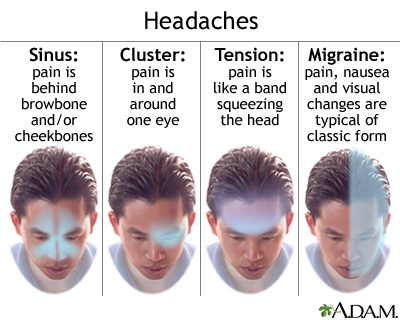
Causes
Tension headaches occur when neck and scalp muscles become tense or contract. The muscle contractions can be a response to stress, depression, head injury, or anxiety.
They may occur at any age, but are most common in adults and older teens. They are slightly more common in women and tends to run in families.
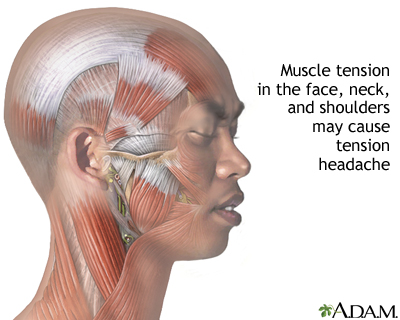
Any activity that causes the head to be held in one position for a long time without moving can cause a headache. Activities may include typing or other computer work, fine work with the hands, and using a microscope. Sleeping in a cold room or sleeping with the neck in an abnormal position may also trigger a tension headache.
Other triggers of tension headaches include:
- Physical or emotional stress
- Alcohol use
- Caffeine (too much or withdrawal)
- Colds, the flu, or a sinus infection
- Dental problems such as jaw clenching or teeth grinding
- Eye strain
- Excessive smoking
- Fatigue or overexertion
Tension headaches can occur when you also have a migraine. Tension headaches are not associated with brain diseases.
Symptoms
The headache pain may be described as:
- Dull, pressure-like (not throbbing)
- A tight band or vise on or around the head
- All over (not just in one point or one side)
- Worse in the scalp, temples, or back of the neck, and possibly in the shoulders
The pain may occur once, constantly, or daily. Pain may last for 30 minutes to 7 days. It may be triggered by or get worse with stress, fatigue, noise, or glare.
You may have difficulty sleeping. Tension headaches usually do not cause nausea or vomiting.
People with tension headaches often try to relieve pain by massaging their scalp, temples, or the bottom of the neck.
Exams and Tests
If your headache is mild to moderate, without other symptoms, and responds to home treatment within a few hours, you may not need to seek medical attention or have further examination or testing.
With a tension headache, there are usually no problems with the nervous system. But tender points (trigger points) in the muscles are often found in the neck and shoulder areas.
Treatment
The goal is to treat your headache symptoms right away and to prevent headaches by avoiding or changing your triggers. A key step in doing this involves learning to manage your tension headaches at home by:
- Keeping a headache diary to help you identify your headache triggers so that you and your health care provider can make changes in your lifestyle to reduce the number of headaches you get
- Learning what to do to relieve a headache when it starts
- Learning how to take your headache medicines the correct way
Many people can treat their tension headaches with conservative therapy, such as relaxation or stress-management training, including:
- Massage
- Biofeedback
- Cognitive behavioral feedback
- Acupuncture
- Ice or hot packs
When needed, medicines that may relieve a tension headache include:
- Over-the-counter (OTC) pain medicines, such as aspirin, ibuprofen, or acetaminophen
- Narcotic pain relievers are generally not recommended
- Muscle relaxers
- Tricyclic antidepressants or certain anti-seizure medicines to prevent recurrences
Be aware that:
- Taking medicines more than 3 days a week may lead to rebound headaches. These are headaches that keep coming back due to overuse of pain medicine.
- Taking too much acetaminophen can damage your liver.
- Too much ibuprofen or aspirin can irritate your stomach or damage your kidneys.
If these medicines do not help, talk to your provider about prescription medicines.
Outlook (Prognosis)
Tension headaches often respond well to treatment. But if the headaches are long-term (chronic), they can interfere with life and work.
When to Contact a Medical Professional
Call 911 or the local emergency number if:
- You are experiencing "the worst headache of your life."
- You have speech, vision, or movement problems or loss of balance, especially if you have not had these symptoms with a headache before.
- The headache starts very suddenly.
- The headache occurs with repeated vomiting.
- You have a high fever or stiff neck with your headache.
Schedule an appointment or contact your provider if:
- Your headache patterns or pain change.
- Treatments that once worked are no longer helpful.
- You have side effects from medicines, including irregular heartbeat, pale or blue skin, extreme sleepiness, persistent cough, depression, fatigue, nausea, vomiting, diarrhea, constipation, stomach pain, cramps, dry mouth, or extreme thirst.
- You are pregnant or could become pregnant. Some medicines should not be taken when pregnant.
- You need to take pain medicines more than 3 days a week.
- Your headaches are more severe when lying down.
Prevention
Learn and practice stress management. Some people find relaxation exercises or meditation helpful. Biofeedback may help you improve the effect of doing relaxation exercises, and may be helpful for long-term (chronic) tension headache.
Tips to prevent tension headaches:
- Keep warm if the headache is associated with cold.
- Use a different pillow or change sleeping positions.
- Practice good posture when reading, working, or doing other activities.
- Exercise the neck and shoulders frequently when working on computers or doing other close work.
- Get plenty of sleep and rest.
Massaging sore muscles may also help.
Alternative Names
Tension-type headache; Episodic tension-type headache; Muscle contraction headache; Headache - benign; Headache - tension; Chronic headaches - tension; Rebound headaches - tension
Patient Instructions
Images
References
Digre KB. Headaches and other head pain. In: Goldman L, Cooney K, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 367.
Garza I, Robertson CE, Smith JH, Whealy MA. Headache and other craniofacial pain. In: Jankovic J, Mazziotta JC, Pomeroy SL, Newman NJ, eds. Bradley and Daroff's Neurology in Clinical Practice. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 102.
Rozental JM. Tension-type headache, chronic tension-type headache, and other chronic headache types. In: Benzon HT, Raja SN, Liu SS, Fishman SM, Cohen SP, eds. Essentials of Pain Medicine. 4th ed. Philadelphia, PA: Elsevier; 2018:chap 20.
Review Date 12/31/2023
Updated by: Joseph V. Campellone, MD, Department of Neurology, Cooper Medical School at Rowan University, Camden, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.