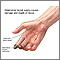
Thromboangiitis obliterans is a rare disease in which blood vessels of the hands and feet become blocked.
Causes
Thromboangiitis obliterans (Buerger disease) causes small blood vessels to become inflamed and swollen. The blood vessels then narrow or get blocked by blood clots (thrombosis). Blood vessels of the hands and feet are mostly affected. Arteries are more affected than veins. Average age when symptoms begin is around 35. Women and older adults are affected less often.
This condition mostly affects men ages 20 to 45 who are heavy smokers or chew tobacco. Female smokers may also be affected. The condition affects more people in the Middle East, Asia, the Mediterranean, and Eastern Europe. Many people with this problem have poor dental health, most likely due to tobacco use.
Symptoms
Symptoms most often affect 2 or more limbs and may include:
- Fingers or toes that appear pale, red, or bluish and feel cold to the touch.
- Sudden severe pain in the hands and feet. The pain may feel like a burning or tingling sensation.
- Pain in the hands and feet that most often occurs when at rest. The pain may be worse when the hands and feet get cold or during emotional stress.
- Pain in the legs, ankles, or feet when walking (intermittent claudication). The pain is often located in the arch of the foot.
- Skin changes or small painful ulcers on the fingers or toes.
- Occasionally, arthritis in the wrists or knees develops before the blood vessels become blocked.
Exams and Tests
The following tests may show blockage of blood vessels in the affected hands or feet:
- Plethysmography exam of the extremity, including pulse volume recording
- Doppler ultrasound of the blood vessels in the extremity
- Catheter-based x-ray arteriogram
Blood tests for other causes of inflamed blood vessels (vasculitis) and blocked (occlusion of) blood vessels may be done. These causes include diabetes, scleroderma, vasculitis, hypercoagulability, and atherosclerosis. There are no blood tests that diagnose thromboangiitis obliterans.
A heart echocardiogram may be done to look for sources of blood clots. In rare cases when the diagnosis is unclear, a biopsy of the blood vessel is done.
Treatment
There is no cure for thromboangiitis obliterans. The goal of treatment is to control symptoms and prevent the disease from getting worse.
Stopping tobacco use of any kind is key to controlling the disease. Smoking cessation treatments are strongly recommended. It is also important to avoid cold temperatures and other conditions that reduce blood flow in the hands and feet.
Applying warmth and doing gentle exercises can help increase circulation.
Aspirin and medicines that open the blood vessels (vasodilators) may help. In very bad cases, surgery to cut the nerves to the area (surgical sympathectomy) can help control pain. Rarely, bypass surgery is considered in certain people.
It may become necessary to amputate the fingers or toes if the area becomes very infected and tissue dies.
Outlook (Prognosis)
Symptoms of thromboangiitis obliterans may go away if the person stops tobacco use. People who continue to use tobacco may need repeated amputations.
Possible Complications
Complications include:
- Tissue death (gangrene)
- Amputation of fingers or toes
- Loss of blood flow in the limb of the affected fingers or toes
When to Contact a Medical Professional
Contact your health care provider if:
- You have symptoms of thromboangiitis obliterans.
- You have thromboangiitis obliterans and symptoms get worse, even with treatment.
- You develop new symptoms.
Prevention
People with a history of Raynaud phenomenon or blue, painful fingers or toes, especially with ulcers, should not use any form of tobacco.
Alternative Names
Buerger disease
References
Akar AR, Ínan MB, SaricaoG?lu MC. Thromboangiitis obliterans. In: Sidawy AN, Perler BA, eds. Rutherford's Vascular Surgery and Endovascular Therapy. 10th ed. Philadelphia, PA: Elsevier; 2023:chap 139.
Bartholomew JR. Other peripheral arterial diseases. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 66.
Bunn C, Halandras PM, Gahtan V. Vascular surgery: Buerger's disease (Thromboangiitis obliterans). In: Cameron J, ed. Current Surgical Therapy. 14th ed. Philadelphia, PA: Elsevier; 2023:993-1214.
Review Date 7/22/2024
Updated by: Neil J. Gonter, MD, Assistant Professor of Medicine, Columbia University, NY and private practice specializing in Rheumatology at Rheumatology Associates of North Jersey, Teaneck, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.