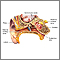
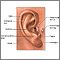
An ear exam is performed when a health care provider looks inside your ear using an instrument called an otoscope.
How the Test is Performed
The provider may dim the lights in the room.
A young child will be asked to lie on their back with the head turned to the side, or the child's head may rest against an adult's chest.
Older children and adults may sit with the head tilted toward the shoulder opposite the ear being examined.
The provider will gently pull up, back, or forward on the ear to straighten the ear canal. Then, the tip of the otoscope will be placed gently into your ear. A light beam shines through the otoscope into the ear canal. The provider will carefully move the scope in different directions to see the inside of the ear and eardrum. Sometimes, this view may be blocked by earwax. An ear specialist may use a binocular microscope to get a magnified look at the ear.
The otoscope may have a plastic bulb on it, which delivers a tiny puff of air into the outer ear canal when pressed. This is done to see how the eardrum moves. Decreased movement of the eardrum can mean that there is fluid in the middle ear.
How to Prepare for the Test
No preparation is needed for this test.
How the Test will Feel
If there is an ear infection, there may be some discomfort or pain. The provider will stop the test if the pain worsens.
Why the Test is Performed
An ear exam may be done if you have an earache, ear infection, hearing loss, or other ear symptoms.
Examining the ear also helps the provider see if treatment for an ear problem is working.
Normal Results
The ear canal differs in size, shape, and color from person to person. Normally, the canal is skin-colored and has small hairs. Yellowish-brown earwax may be present. The eardrum is a light-gray color or a shiny pearly-white. Light should reflect off the eardrum surface.
What Abnormal Results Mean
Ear infections are a common problem, especially with small children. A dull or absent light reflex from the eardrum may be a sign of a middle ear infection or fluid. The eardrum may be red and bulging if there is an infection. Amber liquid or bubbles behind the eardrum are often seen if fluid collects in the middle ear.
Abnormal results may also be due to an external ear infection. You might feel pain when the outer ear is pulled or wiggled. The ear canal may be red, tender, swollen, or filled with yellowish-green pus.
The test may also be done for the following conditions:
- Cholesteatoma
- External ear infection - chronic
- Head injury
- Ruptured or perforated eardrum
Risks
An infection can be spread from one ear to the other if the instrument used to look inside the ear has not been cleaned well.
Considerations
Not all ear problems can be detected by looking through an otoscope. Other ear and hearing tests may be needed.
Otoscopes sold for at-home use are lower quality than the ones used at the provider's office. Parents may not be able to recognize some of the subtle signs of an ear problem. See a provider if there are symptoms of:
- Severe ear pain
- Hearing loss
- Dizziness
- Fever
- Ringing in the ears
- Ear discharge or bleeding
Alternative Names
Otoscopy
References
Murr AH. Approach to the patient with nose, sinus, and ear disorders. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 398.
Wareing MJ, Warner E. Ear, nose and throat. In: Glynn M, Drake WM, eds. Hutchison's Clinical Methods. 25th ed. Philadelphia, PA: Elsevier; 2023:chap 22.
Woodson E, Mowry S. Otologic symptoms and syndromes. In: Flint PW, Francis HW, Haughey BH, et al, eds. Cummings Otolaryngology: Head and Neck Surgery. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 137.
Review Date 3/1/2023
Updated by: Josef Shargorodsky, MD, MPH, Johns Hopkins University School of Medicine, Baltimore, MD. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.